・Review・・Current Issue・ ・Achieve・ ・Search Articles・ ・Online Submission・ ・About IJO・
Ophthalmology
simulation for undergraduate and postgraduate clinical education
Daniel
Shu Wei Ting1,2, Shaun Sebastian Khung Peng Sim1, Christine Wen Leng Yau1, Mohamad Rosman1,2, Ai Tee Aw1, Ian Yew San Yeo1,2
1Third
Hospital Avenue, Singapore
National Eye Centre, 168751, Singapore
2College
Road, DUKE-NUS Medical School Singapore, 169857, Singapore
Correspondence to: Daniel
Shu Wei Ting. Third Hospital Avenue, Singapore National Eye Center, 168751, Singapore. Daniel.ting45@gmail.com
Received: 2015-01-24
Accepted: 2015-09-06
Abstract
This is a review
education paper on the current ophthalmology simulators utilized worldwide for
undergraduate and postgraduate training. At present, various simulators such as
the EYE Exam Simulator (Kyoto Kagaku Co.
Ltd., Kyoto, Japan), Eyesi direct
ophthalmoscope simulator (VRmagic, GmbH, Mannheim, Germany), Eyesi indirect
ophthalmoscope simulator (VRmagic, GmbH, Mannheim, Germany) and Eyesi cataract
simulators (VRmagic, GmbH, Mannheim, Germany). These simulators are thought to
be able to reduce the initial learning curve for the ophthalmology training but
further research will need to be conducted to assess the effectiveness of the
simulation-assisted Ophthalmology training. Future research will be of great
value to assess the medical students and residents’ responses and performance
regarding the usefulness of the individual eye simulator.
KEYWORDS: ophthalmology simulator; cataract simulator; ophthalmology residency
training; direct ophthalmoscopy simulator
DOI:10.18240/ijo.2016.06.22
Citation: Ting DSW, Sim SSKP, Yau CWL, Rosman M,
Aw AT, Yeo IYS. Ophthalmology simulation for undergraduate and
postgraduate clinical education. Int J
Ophthalmol 2016;9(6):920-924
INTRODUCTION
To date, the use
of simulation is becoming increasingly popular in ophthalmology[1]. It
has been shown that technology-enhanced simulation training is associated with
large effects for outcomes of knowledge, skills and behaviors and moderate
effects for patient-related outcomes[2]. In the past,
the clinical teaching was often conducted using real patients and this method
sometimes can be very challenging due to patients’ comfort or time constraint
in a busy clinic. The change of this teaching paradigm mainly arises from
various factors including increased public expectation on doctors’ performance
in diagnosis and management, changes in working practice, advancement in
technological developments and opportunities and shortening of the training
time for the residents.
Due to the
increased health consciousness and awareness in the public, many patients will
research their conditions extensively on the internet prior to their
presentation to the hospital. They often expect the doctors to know what the
immediate clinical findings and diagnoses are instead of being treated as “guinea pigs”
for those who have just entered the residency training or still in the medical
schools. Some of them are often shocked and upset to learn that the examiners
are conducting the clinical examination for the first time on them. The
simulations are good platforms for the medical students and residents to
practice and refine their clinical or surgical technique as they can make
mistakes on simulations without jeopardizing patients’ care[3-4]. It
is a dress rehearsal for a real event, during which mistakes can be made and
lessons learned[5]. Nevertheless,
the simulations should only be used as a method to enhance and supplement the
learning experience as it will not supplant the learning experience from real
patients in the clinical setting[6].
Various forms of
medical simulation such as wet laboratories, mannequins[7],
animal and cadavers[8], simulated
patients, simulated hospital environments, simulated laser or surgical models[9-10],
virtual reality[11-19] are designed to
enhance the students’ and residents’ learning experience. The purpose of this
article is to describe the various ophthalmology simulators that could be
potentially utilized for the medical students and ophthalmology residency
training.
Direct
Fundoscopy Examination Direct
ophthalmoscopy or fundoscopy is a fundus examination skill that has been
incorporated into medical school curriculum as it is an important clinical
skill that allows non-ophthalmology trained physicians to diagnose retinal pathology
without needing to utilize expensive equipment such as slit lamp biomicroscopy
with hand held lends or indirect BIO ophthalmoscopy[20-23]. Through the
direct ophthalmoscopic examination, one can detect many of the
sight-threatening conditions (e.g. proliferative
diabetic retinopathy, glaucomatous optic neuropathy) and life-threatening
conditions (e.g. optic disc swelling
secondary to space occupying lesions, malignant hypertension, meningitis and etc.). However, many students and physicians still had major
difficulties to perform a proficient fundsocopy examination[24-25].
Besides, it is difficult to teach this skill effectively during the initial
phase and for the tutors, it is hard to guide the students while they are
performing the examination due to lack of monitor screen attached to the direct
ophthalmoscope.
Several methods
have been described to supplement the training of medical students in acquiring
this skill. The EYE Exam Simulator (Kyoto Kagaku Co.
Ltd., Kyoto, Japan) is an innovative mannequin
(Figure 1) for fundus examination, designed to allow examination of fundus
using the physician’s own ophthalmoscope. The pupil aperture is adjustable to
simulate both dilated and undilated pupils and the image of the fundus is
created by a set of slides depicting common pathology (Figure 2). The use of
this simulator has been shown to correlate with users’ experience[26] and
the accuracy of the examination decreased with smaller pupil diameters of 2 and
3.5 mm (as opposed to more than 5 mm). It will be of great value to
utilize this device in the practical examination to evaluate direct
ophthalmoscopy skills of medical students and junior residents.

Figure
1 The EYE Exam Simulator (Kyoto Kagaku Co. Ltd., Kyoto, Japan).
Figure
2 Changes of the retinal pathologies using different slides in the EYE Exam
Simulator (Kyoto Kagaku Co. Ltd., Kyoto, Japan).
In addition,
Eyesi direct ophthalmoscope simulator (VRmagic, GmbH, Mannheim, Germany) is a
new device that has recently been released into the market (Figure 3). It uses
virtual reality to enhance the teaching of the essential diagnostic skill of
direct ophthalmoscopy. The simulator has an incorporated curriculum that allows
independent learning by the trainee. It is able to provide prompt feedback on the
user’s view, the examined area and whether the abnormal retinal pathology has
been detected in the simulator. From the monitor screen connected to the direct
ophthalmoscope, the trainer can also evaluate and offer guidance during the
process of examination. In training mode, the findings will be displayed
immediately on the screen as soon as they have been detected and if the trainee
tap on the screen, some relevant information related to the pathology will be
shown. On the other hand, this simulator can also be utilized for assessment
purposes with the quiz mode available in the device and the result can be
generated at the end of the exercise. Whether the skills acquired with the use
of these simulators are translated into clinical practice has yet to be proven.
Further research can be conducted to assess the medical students’ and
physicians’ confidence and competence level in performing direct
ophthalmoscopy. Apart from the abovementioned methods, the Wisconsin School of
Medicine has also described a method for direct ophthalmoscopy training
purposes using a canister or a tin can to simulate an eye-with a fundus photograph stuck to its
base, and a hole drilled into its cap to simulate a pupil[27]. It
has been found to be an inexpensive but effective way in complementing the
direct ophthalmoscopy skills, as compared to the mannequins and Eyesi direct
ophthalmoscope simulators.
Figure
3 Eyesi direct (VRmagic, GmbH, Mannheim, Germany).
Indirect
BIO Ophthalmoscope The
indirect ophthalmoscopy, first devised in 1861 by Felix Giraud Teulon, is an
important diagnostic tool for ophthalmologists. It permits viewing of the
fundus at a wider angle which allows for thorough examination of the peripheral
retina and also viewing through lens opacities. Unlike the direct
ophthalmoscope, the indirect ophthalmoscopy confers binocularity by the use of
mirrors in the instrument to reduce the pupillary distance of the observer to
about 15 mm. The instrument is attached onto a
headband or spectacle frame worn by the examiner, and with the use of a
condensing lens (usually +20 D to
+30 D) held in front of the patient’s eye,
an aerial image of the fundus is formed, magnified, inverted and laterally
reversed. Proficiency in the indirect ophthalmoscopy requires painstaking
practice and junior ophthalmology residents often struggle with maintaining
stability of the instrument and lens and the patient’s eye and difficulty in
lens control[28].
In the past
decades, several training methods, both simple and complex, have been developed
to aid with the training of junior residents in mastering the indirect
ophthalmoscopy[29-30]. A simple
inexpensive setup with the use of a rubber ball or marble held in place by a
Styrofoam head carved out to house a slide holder has been used to simulate the
eye and its anatomic obstacles (e.g.
the eyelids and nose) with the insertion of wide-angle clinical photographs
consisting of various retinal pathologies[31].
More recently,
the Eyesi indirect ophthalmoscope simulator (Figure 4) has been invented to
provide residents with an augmented reality training which encompasses elements
of a physical real-world environment (hand-to-head coordination, anatomic
obstacles) supplemented by a computer generated input (digital fundus
photograph, real-time evaluation andetc)[32]. Eyesi indirect
ophthalmoscope can provide the trainee evaluations of both procedural and
diagnostic skills by assessing the time needed for examination, and percentage
of retina examined properly, which translates into critical information in
assessing a trainee’s proficiency in the indirect ophthalmoscope.

Figure
4 Eyesi indirect
(VRmagic, GmbH, Mannheim, Germany).
It is a good
educational tool given its ability to educate trainees on specific clinical
findings for a given pathology and through a multiple-choice diagnosis
specification tool, trainees are made to describe their findings in detail. The
information captured will then be evaluated by the system for immediate
feedback to the trainee. The information also allows the educator to assess the
trainee’s progress as all performance data is stored in the Eyesi Indirect
database.
Leitritz et al[33] conducted a
study involving 37 medical students with no prior experience in performing
binocular indirect ophthalmoscopy and randomised them into either training in
the conventional way, or with augmented reality ophthalmoscopy (Eyesi
indirect). It has been shown that the group of medical with single training
using the augmented reality ophthalmoscopy is better in improving
ophthalmoscopy skills[33].
Despite the study limitations (small number of students and absence of
crossover design), it holds promise that augmented reality training provides an
efficient learning platform for medical students interested in Ophthalmology
and junior residents. The question, however, remains if the use of such
expensive simulators is translated into measurable clinical advantages and
thus, further studies are required to determine the efficiency and
effectiveness of these simulators and its translation into clinical practice.
Cataract
Simulator Phacoemulsification
training has always been challenging for the junior residents during the
initial period[34-36]. Cataract
simulators have been shown to offer various training advantages to the
ophthalmology residents[37] and these
include shortening the time of feeling confident to operate operation duration[34,38] and
improvement on capsulorrhexis technique[39]. Several types
of cataract simulators are currently available in the market: Eyesi (VRmagic,
GmbH, Mannheim, Germany), PhacoVision (Melerit Medical), and MicrovisTouch
(ImmersiveTouch)[13].
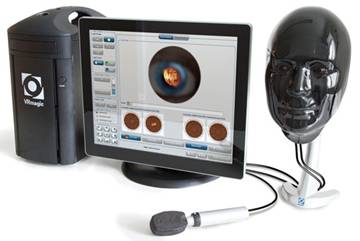
The cataract simulator-Eyesi (VRmagic, GmbH, Mannheim, Germany)
(figure 5) is a high-end virtual reality simulator for intraocular surgical
training and it simulates a life-like learning environment[12,40]. The simulator consists of different
parts including microscope, handheld instruments, a mannequin head with a
virtual eye, foot pedals for microscope and phacoemulsification machine and a
touch-screen monitor on which a supervisor can watch the surgeon perform. For
the hand pieces, they are all colored-coded using optical tracking systems for
conversion of movement to electrical signals then sent to the simulator after
being inserted into the artificial eye. The presence of sophisticated
algorithms in the machine helps to create accurate tissue characteristics and
hence, allowing simulation of procedures such as capsulorrhexis creation[41].

Figure
5 Eyesi cataract simulator (VRmagic, GmbH, Mannheim,
Germany).
In order to offer an immersive surgical simulation
environment, the Eyesi consists of different learning modules including
anti-tremor training, bimanual training, capsulorhexis, cracking and chopping
training, forceps training, hydrodissection maneuvers, intracapsular
anti-tremor training and navigation training, intraocular lens insertion,
irrigation and aspiration, navigation training, phacoemulsification chopping
training and phacoemulsification divide and conquer. The setting of the machine
can also be modified to simulate different surgical environment using various
parameters including phacoemulsification power, vacuum level and flow rate. In
order to assess the residents’ performance on the simulator, the training
history including the number of attempts and the scores for a particular
module, time taken to complete a task, incidence of corneal touch and etc. can be extracted from the machine.
Limited publication is available on Phacovision and
MicrovisTouch. Compared to Eyesi and Phacovision, MircovisTouch, MicrovisTouch
offers users’ tactile feedback interface, hence providing them with more
realistic operative experience[13]. In
addition, it also provides a virtual experience that includes the instruments,
head and eye of the patients. The simulator head and eye in Eyesi and
Phacovision are immobile and this does not simulate the real experience for
cataract surgery.
A recent systematic review showed that the methodology
and validation of various ophthalmology simulators is yet to be improved[8]. Most of the trials did not utilize the
validity of the simulation models for assessment purposes. The efficacy of
training models only satisfy Kirkpatrick model 1 or 2, mainly evaluating the
trainees’ satisfaction with the training model and the extent of the training
increased skills. It is recommended that the skills assessment should be
evaluated using different models with validated scoring system to ensure
appropriate interpretation of results[8].
In conclusion, the use of simulation carries
substantial advantages in the education of medical students and in-training
ophthalmology residents, especially for those who are relatively junior. More
research should be conducted to assess the clinical and cost-effectiveness of
these simulators in enhancing the quality of the clinical service as well as
learning experience of the juniors.
ACKNOWLEDGEMENTS
Conflicts
of Interest: Ting DSW,
None; Sim SSKP, None; Yau CWL, None; Rosman M, None; Aw AT,
None; Yeo IYS, None.
REFERENCES
1 Wallace
BS, Sabates NR. Simulation in ophthalmology. Mo Med 2013;110(2):152-153. [PubMed]
2
Cook DA, Hatala R, Brydges R, Zendejas B, Szostek JH, Wang AT, Erwin PJ,
Hamstra SJ. Technology-enhanced simulation for health professions education: a
systematic review and meta-analysis. JAMA
2011;306(9):978-988. [CrossRef] [PubMed]
3
Gillan SN, Saleh GM. Ophthalmic surgical simulation: a new era. JAMA ophthalmol 2013;131(12):1623-1624. [CrossRef] [PubMed]
4
Grodin MH, Johnson TM, Acree JL, Glaser BM. Ophthalmic surgical training: a
curriculum to enhance surgical simulation. Retina
2008;28(10):1509-1514. [CrossRef] [PubMed]
5 Deanery L. Using simulation in clinical
education. URL: http://www.faculty.londondeanery.ac.uk/e-learning/using-simulation-in-clinical-education.
6
Solverson DJ, Mazzoli RA, Raymond WR, Nelson ML, Hansen EA, Torres MF, Bhandari
A, Hartranft CD. Virtual reality simulation in acquiring and differentiating
basic ophthalmic microsurgical skills. Simul
healthc 2009;4(2):98-103. [CrossRef] [PubMed]
7
Xie P, Hu Z, Zhang X, Li X, Gao Z, Yuan D, Liu Q. Application of 3-dimensional
printing technology to construct an eye model for fundus viewing study. PLoS One 2014;9(11):e109373. [CrossRef] [PubMed] [PMC free article]
8
Thomsen AS, Subhi Y, Kiilgaard JF, la Cour M, Konge L. Update on
simulation-based surgical training and assessment in ophthalmology: a
systematic review. Ophthalmology
2015;122(6):1111-1130.e1. [CrossRef] [PubMed]
9
Moisseiev E, Michaeli A. Simulation of neodymium:YAG posterior capsulotomy for
ophthalmologists in training. J Cataract
Refract Surg 2014;40(2):175-178. [CrossRef] [PubMed]
10
Selvander M, Asman P. Stereoacuity and intraocular surgical skill: effect of
stereoacuity level on virtual reality intraocular surgical performance. J Cataract Refract Surg 2011;37(12):2188-2193. [CrossRef] [PubMed]
11
Colt HG, Crawford SW, Galbraith O 3rd. Virtual reality bronchoscopy simulation:
a revolution in procedural training. Chest
2001;120(4):1333-1339. [CrossRef]
12
Saleh GM, Theodoraki K, Gillan S, Sullivan P, O'Sullivan F, Hussain B, Bunce C,
Athanasiadis I. The development of a virtual reality training programme for
ophthalmology: repeatability and reproducibility (part of the International
Forum for Ophthalmic Simulation Studies). Eye
(Lond) 2013;27(11):1269-1274. [CrossRef] [PubMed] [PMC free article]
13
Sikder S, Tuwairqi K, Al-Kahtani E, Myers WG, Banerjee P. Surgical simulators
in cataract surgery training. Br J
Ophthalmol 2014;98(2):154-158.
[CrossRef] [PubMed]
14
Lowry EA, Porco TC, Naseri A. Cost analysis of virtual-reality
phacoemulsification simulation in ophthalmology training programs. J Cataract Refract Surg 2013;39(10):1616-1617. [CrossRef] [PubMed]
15 Lam CK, Sundaraj K, Sulaiman MN. A systematic
review of phacoemulsification cataract surgery in virtual reality simulators. Medicina (Kaunas) 2013;49(1):1-8.
16
Baxter JM, Lee R, Sharp JA, Foss AJ; Intensive Cataract Training Study Group.
Intensive cataract training: a novel approach. Eye (Lond) 2013;27(6):742-746. [CrossRef] [PubMed] [PMC free article]
17
Yong JJ, Migliori ME, Greenberg PB. A novel preclinical course in ophthalmology
and ophthalmic virtual surgery. Med
Health R I 2012;95(11):345-348.
[PubMed]
18
Le TD, Adatia FA, Lam WC. Virtual reality ophthalmic surgical simulation as a
feasible training and assessment tool: results of a multicentre study. Can J Ophthalmol 2011;46(1):56-60. [CrossRef]
[PubMed]
19
Selvander M, Asman P. Virtual reality cataract surgery training: learning curves
and concurrent validity. Acta Ophthalmol
2012;90(5):412-417. [CrossRef] [PubMed]
20
Ricci LH, Ferraz CA. Simulation models applied to practical learning and skill
enhancement in direct and indirect ophthalmoscopy: a review. Arq Bras Oftalmol 2014;77(5):334-338. [CrossRef] [PubMed]
21
Kelly LP, Garza PS, Bruce BB, Graubart EB, Newman NJ, Biousse V. Teaching
ophthalmoscopy to medical students (the TOTeMS study). Am J Ophthalmol 2013;156(5):1056-1061.e10. [CrossRef] [PubMed] [PMC free article]
22
McCarthy DM, Leonard HR, Vozenilek JA. A new tool for testing and training
ophthalmoscopic skills. J Grad Med Educ 2012;4(1):92-96. [CrossRef] [PubMed] [PMC free article]
23
Podbielski DW, Noble J, Gill HS, Sit M, Lam WC. A comparison of hand- and
foot-activated surgical tools in simulated ophthalmic surgery. Can J Ophthalmol 2012;47(5):414-417. [CrossRef] [PubMed]
24
Wu EH, Fagan MJ, Reinert SE, Diaz JA. Self-confidence in and perceived utility
of the physical examination: a comparison of medical students, residents, and
faculty internists. J Gen Intern Med 2007;22(12):1725-1730. [CrossRef] [PubMed] [PMC free article]
25
Roberts E, Morgan R, King D, Clerkin L. Funduscopy: a forgotten art? Postgrad Med J 1999;75(883):282-284. [CrossRef] [PubMed] [PMC free article]
26
Akaishi Y, Otaki J, Takahashi O, Breugelmans R, Kojima K, Seki M, Komoda T,
Nagata-Kobayashi S, Izumi M. Validity of direct ophthalmoscopy skill evaluation
with ocular fundus examination simulators. Can
J Ophthalmol 2014;49(4):377-381. [CrossRef] [PubMed]
27
Hoeg TB, Sheth BP, Bragg DS, Kivlin JD. Evaluation of a tool to teach medical
students direct ophthalmoscopy. WMJ 2009:108(1):24-26.
[PubMed]
28
Kumar KS, Shetty KB. A new model eye system for practicing indirect
ophthalmoscopy. Indian J Ophthalmol 1996;44(4):233-234. [PubMed]
29
Ing EB, Ing TG. A method of teaching indirect ophthalmoscopy to beginning residents.
Can J Ophthalmol 1992;27(4):166-167. [PubMed]
30
Bartner H, Paton D. An improved model for instruction in binocular indirect
ophthalmoscopy. Arch Ophthalmol 1971;85(5):530-533. [CrossRef] [PubMed]
31
Dodaro NR, Maxwell DP, Jr. An eye for an eye. A simplified model for teaching. Arch Ophthalmol 1995;113(6):824-826. [CrossRef]
32
Schuppe O, Wagner C, Koch F, Manner R. EYESi ophthalmoscope - a simulator for
indirect ophthalmoscopic examinations. Stud
Health Technol Inform 2009;142:295-300. [PubMed]
33
Leitritz MA, Ziemssen F, Suesskind D, Partsch M, Voykov B, Bartz-Schmidt KU,
Szurman GB. Critical evaluation of the usability of augmented reality
ophthalmoscopy for the training of inexperienced examiners. Retina 2014;34(4):785-791. [CrossRef] [PubMed]
34
Pokroy R, Du E, Alzaga A, Khodadadeh S, Steen D, Bachynski B, Edwards P. Impact
of simulator training on resident cataract surgery. Graefes Arch Clin Exp Ophthalmol 2013;251(3):777-781. [CrossRef] [PubMed]
35
Belyea DA, Brown SE, Rajjoub LZ. Influence of surgery simulator training on
ophthalmology resident phacoemulsification performance. J Cataract Refract Surg 2011;37(10):1756-1761. [CrossRef] [PubMed]
36
Ament CS, Henderson BA. Optimizing resident education in cataract surgery. Curr Opin Ophthalmol 2011;22(1):64-67. [CrossRef] [PubMed]
37
Daly MK, Gonzalez E, Siracuse-Lee D, Legutko PA. Efficacy of surgical simulator
training versus traditional wet-lab training on operating room performance of
ophthalmology residents during the capsulorhexis in cataract surgery. J Cataract Refract Surg 2013;39(11):1734-1741. [CrossRef] [PubMed]
38
Selvander M, Asman P. Ready for OR or not? Human reader supplements Eyesi
scoring in cataract surgical skills assessment. Clin Ophthalmol 2013;7:1973-1977. [CrossRef] [PubMed] [PMC free article]
39
McCannel CA, Reed DC, Goldman DR. Ophthalmic surgery simulator training
improves resident performance of capsulorhexis in the operating room. Ophthalmology 2013;120(12):2456-2461. [CrossRef] [PubMed]
40
Selvander M, Asman P. Cataract surgeons outperform medical students in Eyesi
virtual reality cataract surgery: evidence for construct validity. Acta Ophthalmol 2013;91(5):469-774. [CrossRef] [PubMed]
41
Grimm J. Tearing of membranes for interactive real-time surgical training. Stud Health Technol Inform 2005;111:153-159. [PubMed]
[Top]
