INTRODUCTION
Corneal collagen cross-linking (CXL) is a method aime at increasing the number of bonds between the collagen chains of the corneal stroma, thus inducing a change in the mechanical properties of the cornea[1]. This technique has been shown to be effective in the fi eld of corneal ectasia, preventing its progression and even regularising the corneal surface in these cases[1-6]. The need for epithelial debridement of the cornea to obtain a sufficient degree of riboflavin penetration and consequently a greater cross-linking effect was one of the main initial drawbacks of the CXL technique, as it prolonged the recovery and increased postoperative discomfort[7]. For this reason, new CXL protocols are being developed in order to avoid having to debride the corneal epithelium, such as transepithelial CXL[7].
SUBJECTS AND METHODS
This prospective, randomised study evaluated a total of 19 keratoconus eyes of 12 patients aged between 26 and 69y undergoing accelerated transepithelial CXL. All patients belonged to the Corneal and Anterior Segment Unit of the Ophthalmology Department (OFTALMAR), Vithas Medimar International Hospital (Alicante, Spain). The study inclusion criterion was the presence of progressive keratoconus:central topographic steepening of more than 1 diopters (D)with refractive change of more than 0.50 D in the last 6mo.The standard criterion for diagnosing keratoconus was used:corneal topography showing an asymmetric bow-tie pattern with or without inclined axes and at least one keratoconic sign on slit-lamp examination, such as stromal thinning, conic protrusion of the cornea atthe apex, Fleischer's ring, Vogt's striae or anterior stromal scarring. The exclusion criteria were previous eye surgery and the presence of any type of active eye disease. All patients were properly informed about their inclusion and signed an informed consent form. The study complied with the principles of the Declaration of Helsinki,and was approved by the Hospital Ethics Committee.
A complete ophthalmological examination was carried out preoperatively, which included measurement of manifest refraction, uncorrected distance visual acuity (UDVA) and corrected distance visual acuity (CDVA), Goldmann applanation tonometry, anterior segment slit-lamp examination, corneal topography and aberrometry (Sirius, CSO, Florence, Italy),optical biometry and eye fundus examination. Postoperatively,patients were reviewed 1d, 1, 6 and 12mo post-surgery. The day after the surgery, a biomicrosopic examination of the cornea was carried out, as well as an analysis of the cornea by optical coherence tomography (OCT; 3D-1000 system,Topcon), measuring the depth of the area of highest ref l ectance(corneal demarcation line). The same examination protocol as in the preoperative period was used at 1, 6 and 12mo.
Table 1 Summary of the visual, refractive, corneal topographic and pachymetric outcomes in the analyzed sample
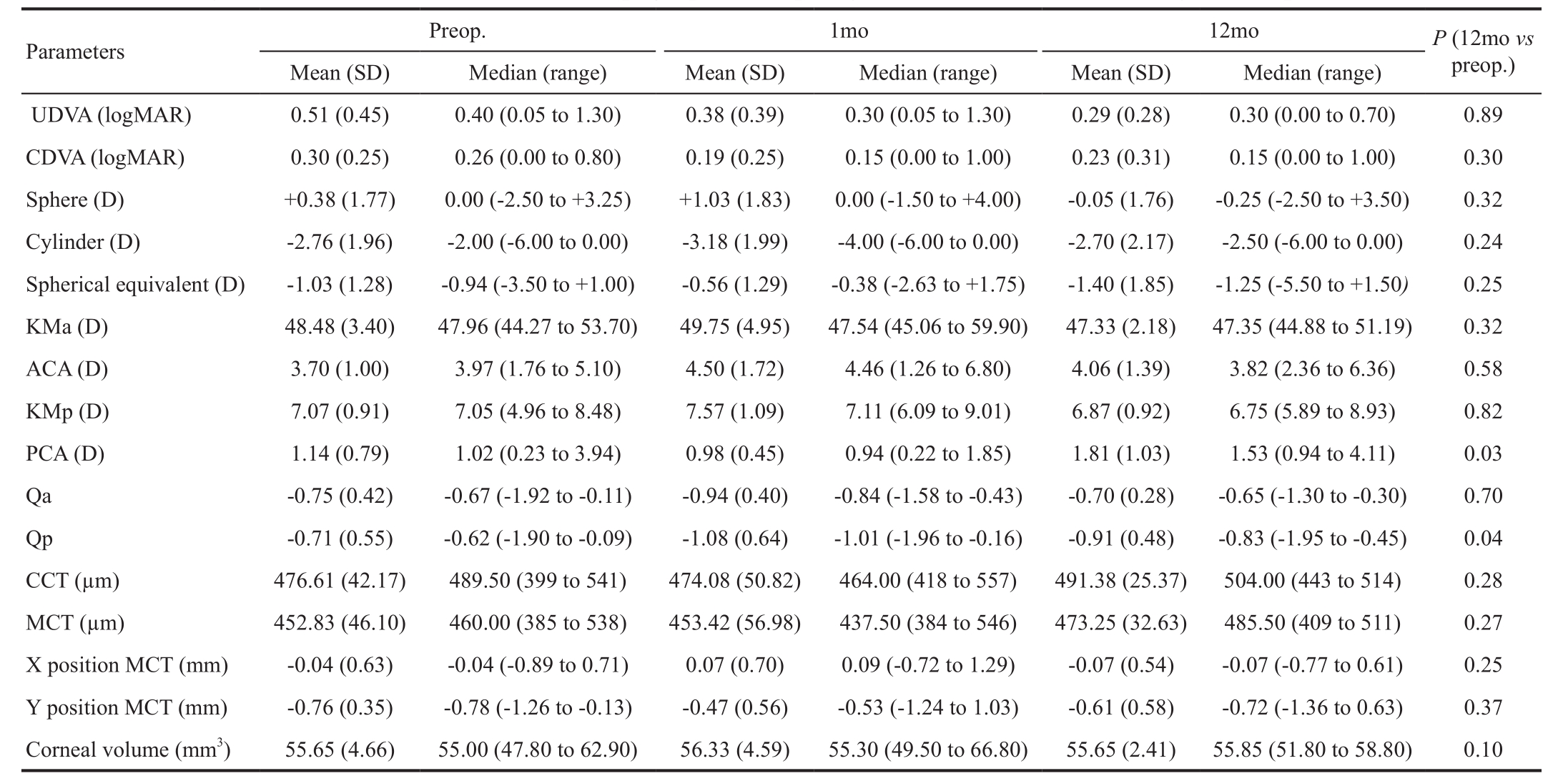
SD: Standard deviation; D: Diopters; UDVA: Uncorrected distance visual acuity; CDVA: Corrected distance visual acuity; KMa: Anterior mean keratometry;ACA: Anterior corneal astigmatism in the 3-mm central area; KMp: Posterior mean keratometry; PCA: Posterior corneal astigmatism in the 3-mm central area; Qa: Asphericity of the anterior corneal surface in the central 8-mm area; Qp: Asphericity of the posterior corneal surface in the central 8-mm area; CCT:Central corneal thickness; MCM: Minimal corneal thickness.
All operations were performed by the same expert surgeon(Artola A) under topical anaesthesia, using the Avedro KXL cross-linking system (Waltham, MA, USA). The procedure began with the instillation, every 90s for a total of 4min, of dextran-free hypo-osmolar ribof l avin drops containing agents to improve the epithelial permeability, including benzalkonium chloride (Paracel, Avedro, Waltham, MA, USA). A benzalkonium chloride-free 0.25% riboflavin solution (VibeXXtra, Avedro,Waltham, MA, USA) was then instilled at the same rate for 6min. Once these steps had been completed, ultraviolet radiation was applied for 2min and 40s, using a pulsed light protocol(2s ON /1s OFF). The total energy irradiated was 7.2 J/cm2 and the ultraviolet power was 45 mW/cm2. After irradiation, the cornea was rinsed with balanced saline solution.
RESULTS AND DISCUSSION
One month after surgery, a non-statistically signif i cant change was noted in sphere (Ρ=0.18) and in spherical equivalent(Ρ=0.17), with no associated significant changes in cylinder(Ρ=0.65) or logMAR UDVA (Ρ=0.26). Likewise, a slight but statistically significant difference was observed in logMAR CDVA at 1mo postoperatively (Ρ=0.04). There were no signif i cant changes in either visual acuity or refraction between 1 and 12mo (Ρ≥0.40) (Table 1).
Table 1 shows also a summary of the corneal topography changes observed post-operatively. Only a statistically signif i cant changed with surgery was observed in the magnitude of the astigmatism of the posterior surface (Ρ=0.03) and in posterior corneal asphericity (Ρ=0.04). Regarding corneal aberrations,no signif i cant changes were noted at 1mo post-surgery (Ρ≥0.09)or in the remaining follow-up (Ρ≥0.08; Table 2).
Finally, the mean depth of the demarcation line measured by OCT varied between 153 and 230 µm, with a mean value of 205.19 µm (SD: 19.75; median: 205 µm).
In this study, we observed that the accelerated transepithelial CXL technique induces variable changes in the spherical defect and spherical equivalent of the patient. Thus, changes in the mechanical properties of the cornea induced by crosslinking seem to produce a change in the optical properties of the cornea, eventually affecting the refractive level. This is consistent with the fi ndings reported in other series evaluating the results of transepithelial CXL, either by iontophoresis or accelerated[8-12]. Similarly, in line with all previous studies on transepithelial CXL[8-12], a significant improvement in CDVA was observed after surgery that remained throughout the entire 12mo follow-up period.
As regards topographic changes after CXL, central fl attening of the anterior corneal surface was observed in our series,which did not reach statistical significance. No significant changes were noted either in the curvature of the posterior corneal surface during the 12-month follow-up period, or in the asphericity of the anterior surface. A statistically signif i cant change towards more negative asphericity values was observed for the posterior corneal surface. Lesniak and Hersh[10] found a mean reduction of 0.9 D in the maximum keratometry in a prospective study that evaluated the results of a similar CXL technique than that used in our study over a 6mo period. It should be borne in mind that this study included keratoconus cases that were more advanced than in our series, so the mean keratometry was higher. However, a statistically significant change was observed in the magnitude of the astigmatism of the posterior surface between 1 and 12mo after surgery,causing an increase in this value. This could be indicative of more long-term changes in the corneal structure after CXL.The different degrees of ribof l avin penetration from one eye to another may also have played a crucial role in the variability of the CXL effect. More complex studies are therefore required that characterise the in vivo changes at the biomechanical level of the cornea structure, as have already been studied ex vivo[13].With respect to corneal aberrations, as with the topographic parameters, there was wide inter-patient variability, with no statistically signif i cant changes.
Table 2 Summary of the corneal aberrometric outcomes in the analyzed sample
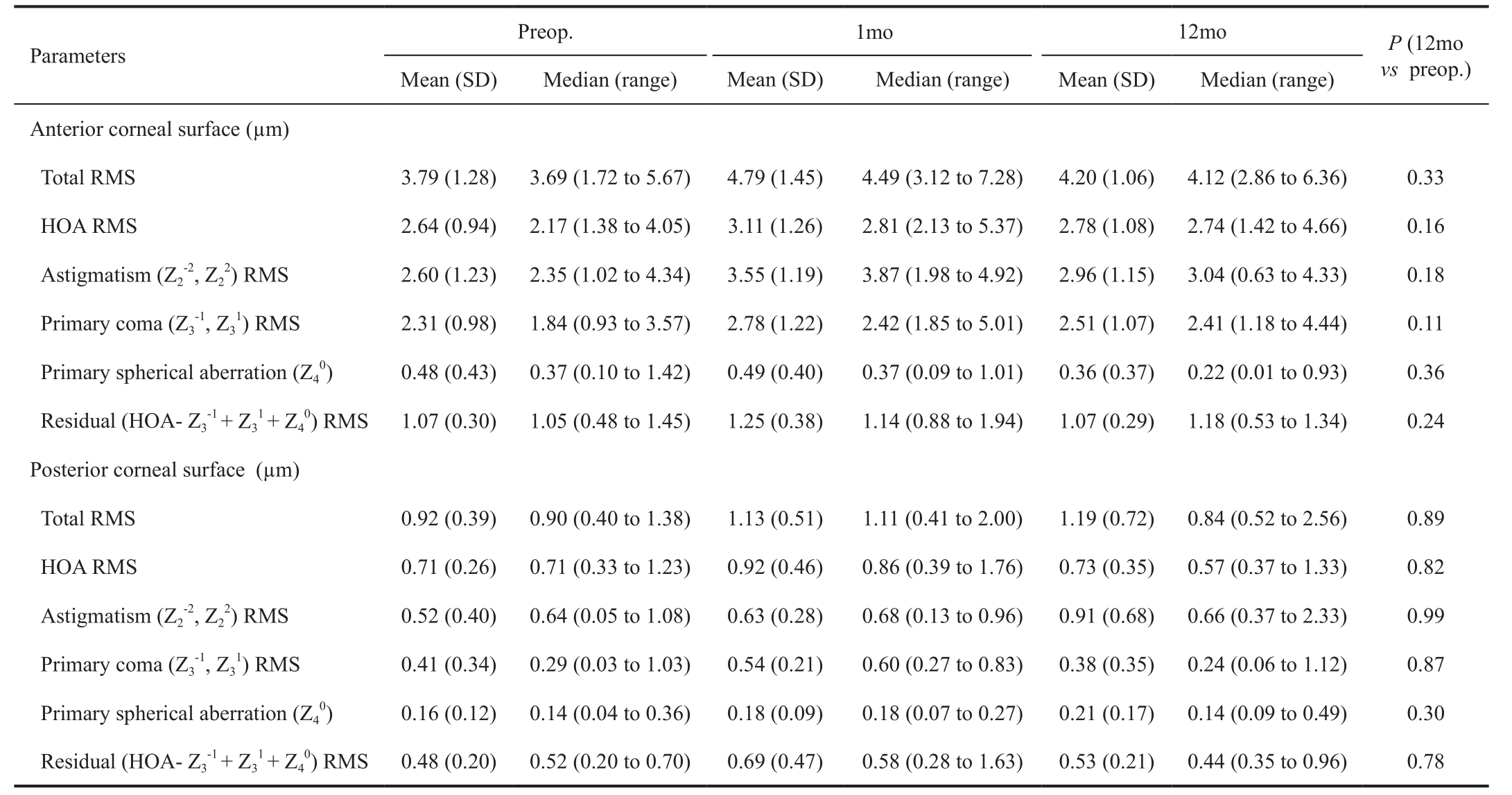
SD: Standard deviation; RMS: Root mean square; HOA: Higher order aberration.
The central and minimum pachymetry underwent changes, but they did not reach statistical significance. A non-significant trend towards a reduction in pachymetric values was observed 1mo after the surgery, with thickening at 12mo. Similar trends were reported by Nawaz et al[14] comparing patients with keratoconus undergoing conventional or transepithelial CXL.Finally, the corneal demarcation line measured by OCT had a mean depth of 202.72 µm, which is consistent with the degree of ribof l avin penetration measured in experimental studies that have evaluated the effect of transepithelial CXL[15].In summary, accelerated transepithelial CXL could be a potentially useful technique for the management of progressive corneal ectasia, as it can maintain the topographic and aberrometric prof i le of the cornea without signif i cant changes for a period of 12mo after the procedure. Future studies are warranted that show the corneal biomechanical changes that occur in-vivo with the use of this technique.
ACKNOWLEDGEMENTS
Conflicts of Interest: Artola A, None; Piñero DP, None;Ruiz-Fortes P, None; Soto-Negro R, None; Pérez-Cambrodí RJ, None.
REFERENCES
1 O'Brart DPS. Corneal collagen cross-linking: A review. J Optom 2014;7(3):113-124.
2 Chow VW, Chan TC, Yu M, Wong VW, Jhanji V. One-year outcomes of conventional and accelerated collagen crosslinking in progressive keratoconus. Sci Rep 2015;5:14425.
3 Ghanem RC, Santhiago MR, Berti T, Netto MV, Ghanem VC.Topographic, corneal wavefront, and refractive outcomes 2 years after collagen crosslinking for progressive keratoconus. Cornea 2014;33(1):43-48.
4 Asri D, Touboul D, Fournié P, Malet F, Garra C, Gallois A, Malecaze F, Colin J. Corneal collagen crosslinking in progressive keratoconus:multicenter results from the French National Reference Center for Keratoconus. J Cataract Refract Surg 2011;37(12):2137-2143.
5 Hafezi F, Kanellopoulos J, Wiltfang R, Seiler T. Corneal collagen crosslinking with ribof l avin and ultraviolet A to treat induced keratectasia after laser in situ keratomileusis. J Cataract Refract Surg 2007;33(12):2035-2040.
6 Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-a-induced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol 2003;135(5):620-627.
7 Wollensak G, Iomdina E. Biomechanical and histological changes after corneal crosslinking with and without epithelial debridement. J Cataract Refract Surg 2009;35(3):540-546.
8 Elbaz U, Shen C, Lichtinger A, Zauberman NA, Goldich Y, Ziai S,Rootman DS. Accelerated versus standard corneal collagen crosslinking combined with same day phototherapeutic keratectomy and single intrastromal ring segment implantation for keratoconus. Br J Ophthalmol 2015;99(2):155-159.
9 Mazzotta C, Traversi C, Caragiuli S, Rechichi M. Pulsed vs continuous light accelerated corneal collagen crosslinking: in vivo qualitative investigation by confocal microscopy and corneal OCT. Eye (Lond)2014;28(10):1179-1183.
10 Lesniak SP, Hersh PS. Transepithelial corneal collagen crosslinking for keratoconus: six-month results. J Cataract Refract Surg 2014;40(12):1971-1979.
11 Caporossi A, Mazzotta C, Paradiso AL, Baiocchi S, Marigliani D,Caporossi T. Transepithelial corneal collagen crosslinking for progressive keratoconus: 24-month clinical results. J Cataract Refract Surg 2013;39(8):1157-1163.
12 Spadea L, Mencucci R. Transepithelial corneal collagen crosslinking in ultrathin keratoconic corneas. Clin Ophthalmol 2012;6:1785-1792.
13 Lombardo M, Serrao S, Rosati M, Ducoli P, Lombardo G. Biomechanical changes in the human cornea after transepithelial corneal crosslinking using iontophoresis. J Cataract Refract Surg 2014;40(10):1706-1715.
14 Nawaz S, Gupta S, Gogia V, Sasikala NK, Panda A. Trans-epithelial versus conventional corneal collagen crosslinking: a randomized trial in keratoconus. Oman J Ophthalmol 2015;8(1):9-13.
15 Bouheraoua N, Jouve L, El Sanharawi M, Sandali O, Temstet C,Loriaut P, Basli E, Borderie V, Laroche L. Optical coherence tomography and confocal microscopy following three different protocols of corneal collagen-crosslinking in keratoconus. Invest Ophthalmol Vis Sci 2014;55(11):7601-7609.