
・Meta-Analysis・ Current
Issue IF in JCR CiteScore ・Submission・ In Press Recent Accepted PMC RSS
Citation:
Maroufizadeh S, Almasi-Hashiani A, Omani Samani R, Sepidarkish M. Prevalence of
retinopathy of prematurity in Iran: asystematic review and Meta-analysis. Int
J Ophthalmol 2017;10(8):
1273-1279
Prevalence of retinopathy of prematurity in Iran:
asystematic review and Meta-analysis
Saman Maroufizadeh, Amir Almasi-Hashiani, Reza
Omani Samani, Mahdi Sepidarkish
Department
of Epidemiology and Reproductive Health, Reproductive Epidemiology Research
Center, Royan Institute for Reproductive Biomedicine, ACECR, Tehran 16635-148,
Iran
Correspondence to: Reza Omani Samani.
Department of Epidemiology and Reproductive Health, Reproductive Epidemiology
Research Center, Royan Institute for Reproductive Biomedicine, ACECR, Tehran
16635-148, Iran. samani@royaninstitute.org
Received: 2016-07-29
Accepted: 2017-01-13
Abstract
AIM:
To estimate overall prevalence of retinopathy of prematurity (ROP) in Iran
using a systematic review and Meta-analysis.
METHODS:
A systematic review and Meta-analysis was performed of all published studies
pertaining to prevalence of ROP using international and national electronic
databases (ISI Web of Sciences, PubMed, Scopus, Google Scholar, SID, MagIran,
and IranMedex) from their inception until May 2016 with standard keywords. Begg
and Egger tests were used to examine the publication bias and Cochran test and I2
statistics were used to evaluate the statistical heterogeneity. Pooled estimate
of the prevalence of ROP were calculated using random effects Meta-analysis.
RESULTS: The
publication bias assumption was rejected by Egger tests with P-value
equal to 0.024. The results of Cochran test and I2 statistics
revealed substantial heterogeneity (Q=1099.02, df=25, I2=97.7%,
P=0.001). The overall prevalence of ROP using the random effect model in
Iran was 26.1% (95% CI: 20.3%-31.8%).
CONCLUSION: The
prevalence of ROP is relatively high in Iran. Low birth weight and gestational
age are significant risk factors for the disease. Improved care, including
oxygen delivery and monitoring, for preterm babies in all facility settings
would reduce the number of babies affected with ROP.
KEYWORDS: retinopathy
of prematurity; preterm birth; infant; Meta-analysis; systematic review; Iran
DOI:10.18240/ijo.2017.08.15
Citation: Maroufizadeh S, Almasi-Hashiani A, Omani Samani R, Sepidarkish M.
Prevalence of retinopathy of prematurity in Iran: asystematic review and Meta-analysis.
Int J Ophthalmol 2017;10(8):
1273-1279
INTRODUCTION
Retinopathy of prematurity (ROP), previously known as retrolental
fibroplasia, is a proliferative vascular disorder of the retina that can lead
to poor visual acuity or blindness in preterm infants[1].
It affects a substantial number of preterm infants and is a leading cause of
potentially preventable childhood blindness throughout the world[2]. Moreover, the increased survival of preterm infants in
recent years, due to improvement in antenatal and neonatal care, has produced a
population of infants at high risk of developing ROP[2].
The two most important risk factors for developing ROP are low birth weight
(BW) and low gestational age (GA)[3-5].
Other risk factors include oxygen therapy, sex, sepsis, anemia,
intraventricular hemorrhage and blood transfusion[3-4,6-9].
Numerous studies have been conducted to determine the prevalence of ROP
and its related factors in Iran. However, there is a remarkable diversity among
the results. The prevalence of ROP in these studies was between 5.6% and 70.3%[10-35].
Due to the substantial heterogeneity among the reported prevalence and
the importance of prevention and treating ROP, which constitutes a major burden
for health care systems, the accurate determination of ROP prevalence is
essential for strategic plan and health policy. Given the importance of the
subject, we performed a systematic review and Meta-analysis of all published
studies pertaining to prevalence of ROP in Iran.
MATERIALS AND METHODS
Search Strategy and Study Selection Criteria To collect related articles, both international and national databases
including ISI Web of Sciences, PubMed, Scopus, Google Scholar, SID, MagIran,
and IranMedex were searched for MeSH terms “retinopathy of prematurity”, “ROP”
and “Iran” and their Persian equivalents in titles or abstracts. A systematic
review in the mentioned database was done without any time restriction.
Duplications, Meta-analysis and case reports were excluded from analysis.
All Persian or English included studies were cross-sectional study
(descriptive or analytical). All records were included in Endnote X6 for
assessing and categorizing. At the first, title and abstract were
systematically assessed for finding the relevant studies. Then, eligible
studies were obtained for full text screening. All relevant publications were
separately reviewed by two reviewers (Maroufizadeh S and Almasi-Hashiani A) for
the eligibility criteria. Disagreement between reviewers was resolved by
consensus.
Data Extraction and Study Quality
After review of the full texts, the
following data were extracted from each study: study and participant
characteristics including first author’s name, date of study, sample size,
province or city of the study, BW, GA, boy/girl (B/G) ratio, year of
publication and ROP prevalence. The quality of the studies was evaluated using
a modified STROBE checklist.
Data Analysis All statistical analyses were performed using Stata version 13.0
(StataCorp, College Station, TX, USA). The prevalence of ROP was polled by the
“metan” command and showed by a forest plot. The Cochrane Q test and I2
statistic were used to test heterogeneity across studies[36].
A P-value <0.1, rather than <0.05, was used as evidence of
heterogeneity for the Cochrane Q test, as recommended by the Cochrane
Collaboration. The I2 statistic expresses the percentage of
total variation across studies due to heterogeneity. I2
values of 25%, 50% and 75% correspond to low, moderate and high heterogeneity,
respectively[36]. Considering the substantial
heterogeneity among studies, we used a random effects model for all analyses.
Meta regression was used to explore the sources of between-study heterogeneity,
including year of study, sample size, BW, GA and sex ratio. Moreover, the
Galbraith plot was used to detect the potential sources of heterogeneity[37]. The Funnel plot and Begg's rank correlation and
Egger's weighted regression tests were used to assess publication bias by
“metabias” command[38-39]. To
correct publication bias, the Trim and Filled method was used by the “metatrim”
command in Stata. Sensitivity analysis was done by “metainf” command.
RESULTS
The findings of this review are summarized in Table 1. We include 26
individual studies from 10 provinces across the country (with 8786 cases). All
included papers were cross-sectional studies. The sample size of the studies
was between 50 and 1053 cases. The study flowchart was show in Figure 1.
Table
1 Description of the studies included in the Meta-analysis
|
Authors |
Location |
Year |
n |
Prevalence
(%) |
Inclusion
criteria [GA (wk); BW (g)] |
GA (wk) |
BW (g) |
B/G ratio |
|
Riazi
Esfahani et al[10] |
Tehran |
1997-1999 |
150 |
6.0 |
GA≤37 or
BW≤2500 |
33.46 |
1814.5 |
0.97 |
|
Nakshab
et al[11] |
Sari |
2001-2002 |
68 |
11.8 |
BW≤2500 |
32.30 |
1695.9 |
NR |
|
Karkhaneh
et al[12] |
Tehran |
2000-2002 |
185 |
12.4 |
GA≤37 or
BW≤2500 |
31.64 |
1620.7 |
1.47 |
|
Mansouri
et al[13] |
Tehran |
2004-2005 |
147 |
29.9 |
GA≤32;
BW≤1500 |
30.30 |
1385.8 |
1.01 |
|
Karkhaneh
et al[14] |
Tehran |
2003-2007 |
953 |
34.5 |
GA≤37 |
31.10 |
1542.0 |
1.19 |
|
Fayyazi
et al[15] |
Tabriz |
2005-2006 |
399 |
7.3 |
GA≤37 or
BW≤2500, and infant with BW: 1500-2500 who had unstable condition |
NR |
NR |
NR |
|
Khatami
et al[16] |
Mashhad |
2000-2001 |
50 |
28.0 |
GA≤34;
BW≤2000 |
32.86 |
1586.0 |
0.92 |
|
Mousavi
et al[17] |
Tehran |
2001-2006 |
191 |
39.3 |
Premature
infants with late retinal examination |
30.00 |
1404.0 |
1.15 |
|
Riazi-Esfahani
et al[18] |
Tehran |
2002-2004 |
198 |
13.6 |
GA≤30 or
BW≤2500 |
32.04 |
1635.4 |
1.08 |
|
Sadeghi
et al[19] |
Tabriz |
NR |
150 |
17.3 |
GA≤36;
BW≤2000 |
29.12 |
1438.7 |
1.27 |
|
Fouladinejad
et al[20] |
Gorgan |
2004-2005 |
89 |
5.6 |
GA≤34 |
NR |
NR |
1.02 |
|
Mousavi
et al[21] |
Tehran |
2001-2007 |
216 |
40.3 |
Infants
with late retinal examination |
29.90 |
1410.0 |
1.25 |
|
Naderian
et al[22] |
Isfahan |
2002-2008 |
796 |
16.8 |
25≤GA≤34;
600≤BW≤1800 |
29.50 |
1300.0 |
1.04 |
|
Saeidi
et al[23] |
Mashhad |
2005-2006 |
47 |
8.5 |
GA≤32;
BW≤1500 |
NR |
1223.7 |
0.96 |
|
Bayat-Mokhtari
et al[24] |
Shiraz |
2006-2007 |
199 |
42.2 |
BW<1500
or infants with BW between 1500-2000 who had unstable clinical condition |
30.80 |
1393.1 |
1.14 |
|
Mousavi
et al[25] |
Tehran |
2003-2007 |
1053 |
36.1 |
Premature
infants |
NR |
NR |
NR |
|
Naderian
et al[26] |
Isfahan |
2003-2008 |
604 |
17.5 |
GA≤37;
BW≤2500 |
31.00 |
1375.3 |
1.16 |
|
Ebrahim
et al[27] |
Babol |
2004-2008 |
173 |
19.1 |
GA≤37 |
32.24 |
1680.6 |
1.06 |
|
Ghaseminejad
and Niknafs[28] |
Kerman |
2006-2008 |
83 |
28.9 |
GA≤36;
BW≤2500 |
31.76 |
1543.4 |
1.44 |
|
Naderian
et al[29] |
Isfahan |
NR |
200 |
35.5 |
GA≤34;
BW≤1800 |
30.72 |
1325.5 |
1.00 |
|
Afarid
et al[30] |
Shiraz |
2006-2010 |
787 |
37.2 |
GA≤32 or
BW≤2000 |
30.87 |
1397.0 |
0.98 |
|
Feghhi
et al[31] |
Ahvaz |
2006-2010 |
576 |
31.8 |
GA≤32
and/or BW≤2500 |
31.64 |
1204.0 |
1.09 |
|
Abrishami
et al[32] |
Mashhad |
2006-2010 |
122 |
26.2 |
GA≤32 |
30.54 |
1249.0 |
0.88 |
|
Sabzehei
et al[33] |
Tehran |
2007-2010 |
414 |
17.1 |
BW≤1500 |
30.45 |
1268.6 |
1.01 |
|
Ahmadpour-kacho
et al[34] |
Babol |
2009-2012 |
256 |
70.3 |
GA≤28;
BW≤1500; infant with GA: 29-34 and BW:1500-2000 with an unstable clinical
condition |
31.08 |
1489.6 |
0.98 |
|
Rasoulinejad
and Montazeri[35] |
Babol |
2007-2013 |
680 |
45.0 |
GA≤37 or
BW≤2500 |
31.45 |
1713.9 |
1.66 |
GA:
Gestational age; BW: Birth weight; B/G ratio: Boy/girl ratio; NR: Not reported.
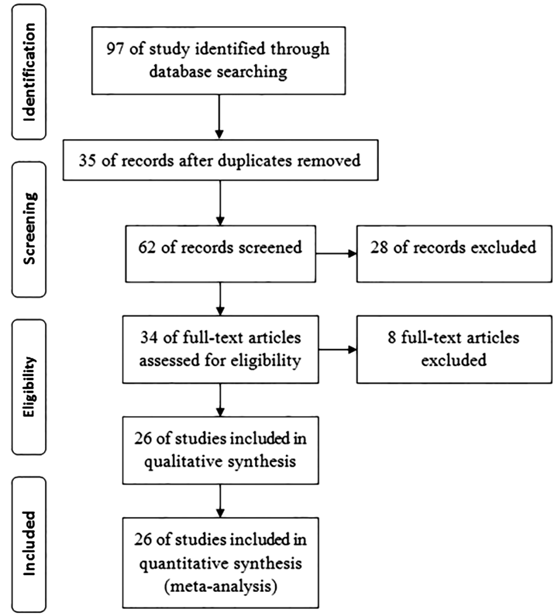
Figure 1 Study flowchart.
The results of Cochran’s Q test and I2 statistics
showed high heterogeneity among the included studies. Due to evidence of
heterogeneity in studies (Q=1099.02, df=25, I2=97.7%, P=0.001),
random model was used to poll the studies. The overall estimates of the
prevalence of ROP based on the individual studies were 26.1% (95% CI:
20.3%-31.8%) (Figure 2). The highest prevalence of ROP (70.3%, 95% CI:
64.7%-75.9%) was reported from Babolcity, and the lowest prevalence of ROP
(5.6%, 95% CI: 0.8%-10.4%) was reported in Golestan Province.
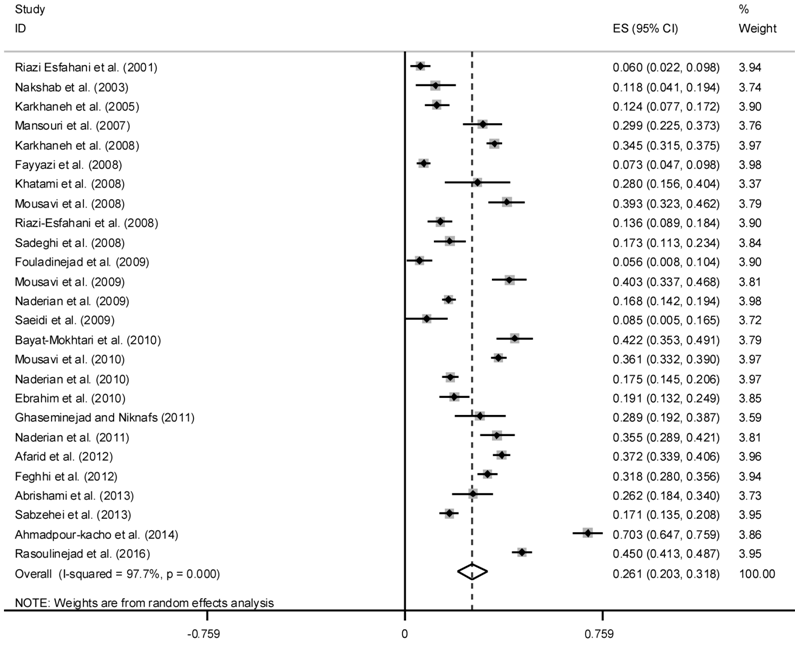
Figure 2 Prevalence of ROP in Iranian neonatal.
Meta-regression for Heterogeneity
Meta regression was used to explore the
sources of between-study heterogeneity, including year of publication, sample
size, BW, GA and B/G ratio. This analysis revealed that the year of publication
is responsible for heterogeneity. Therefore, a cumulative Meta-analysis and
subgroup analysis based on the year of publication were performed. In the
subgroup analysis, the individual studies were divided into two time periods of
publication, before and after 2010. The polled estimated prevalence of ROP
before and after 2010 were different, 19.2 (95% CI: 12.8-25.5) and 33.9 (95%
CI: 26.1-41.8), respectively. After running cumulative Meta-analysis with
“metacum” command in Stata, the prevalence of ROP showed an increase from 6.0%
in 2001 to 24.1% in 2016 (Figure 3). Also we perform sensitivity analysis to
identify the effect of the each study on polled estimate and the results showed
that Ahmadpour-kacho et al[34] study has
more effect on polled estimate so that after removing it the polled estimate
decreases to 24.2% (Table 2).
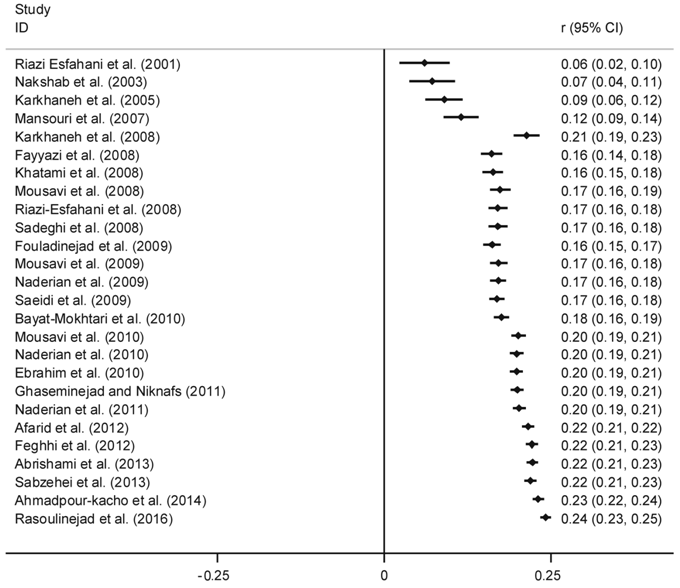
Figure 3 Cumulative prevalence of ROP according to year of publication.
Table 2 Sensitivity analysis to identify the effect of each study on
polled estimate
|
Authors |
Prevalence
(95% CI) |
|
Riazi
Esfahani et al[10] |
0.269
(0.211-0.326) |
|
Nakshab
et al[11] |
0.266
(0.208-0.324) |
|
Karkhaneh
et al[12] |
0.266
(0.207-0.325) |
|
Mansouri
et al[13] |
0.259
(0.200-0.318) |
|
Karkhaneh
et al[14] |
0.257
(0.198-0.316) |
|
Fayyazi
et al[15] |
0.268
(0.212-0.325) |
|
Khatami
et al[16] |
0.260
(0.201-0.318) |
|
Mousavi
et al[17] |
0.255
(0.197-0.314) |
|
Riazi-Esfahani
et al[18] |
0.266
(0.207-0.324) |
|
Sadeghi
et al[19] |
0.264
(0.205-0.323) |
|
Fouladinejad
et al[20] |
0.269
(0.211-0.327) |
|
Mousavi
et al[21] |
0.255
(0.197-0.313) |
|
Naderian
et al[22] |
0.264
(0.204-0.325) |
|
Saeidi
et al[23] |
0.267
(0.209-0.326) |
|
Bayat-Mokhtari
et al[24] |
0.254
(0.196-0.312) |
|
Mousavi
et al[25] |
0.256
(0.197-0.315) |
|
Naderian
et al[26] |
0.264
(0.204-0.324) |
|
Ebrahim
et al[27] |
0.263
(0.204-0.322) |
|
Ghaseminejad
and Niknafs[28] |
0.259
(0.201-0.318) |
|
Naderian
et al[29] |
0.257
(0.198-0.315) |
|
Afarid
et al[30] |
0.256
(0.197-0.315) |
|
Feghhi
et al[31] |
0.258
(0.199-0.318) |
|
Abrishami
et al[32] |
0.260
(0.202-0.319) |
|
Sabzehei
et al[33] |
0.264
(0.204-0.324) |
|
Ahmadpour-kacho
et al[34] |
0.243
(0.191-0.294) |
|
Rasoulinejad
and Montazeri[35] |
0.253
(0.196-0.309) |
|
Combined |
0.261
(0.203-0.318) |
CI:
Confidence interval.
Publication Bias Begg’s test, Egger’s test and also Funnel plot were used to determine
the present of publication bias and there was a controversy between Begg’s and
Egger’s tests (P=0.582, 0.024, respectively), and based on Begg’s test
there was no evidence of publication bias but Egger’s test shows some evidence
of publication bias in the studies. Since the Egger’s test has more power,
therefore, the Trim and Filled method was used to estimate the prevalence of
ROP. By Trim and Filled analysis, ROP prevalence in Iran was estimated as 20.9%
(95% CI: 14.8%-27.1%).
DISCUSSION
The
major goal of the present study was to estimate the prevalence of ROP in Iran.
Based on the results of the Meta-analysis, the prevalence of ROP in Iran was
estimated to be 26.1% (95% CI: 20.3%-31.8%). In the Meta-analysis, the larger
sample size will be reviewed and estimation would be more accurate for
researchers and policy makers[40]. In Iran, the
prevalence of ROP in published papers was reported between 5.6% and 70.3%[10-35], after weighting for each study
we polled these studies.
ROP
is a potentially blinding disease of the retina. In spite of in progress
screening and different treatment guidelines, ROP is still a main cause of
blindness in children in the both developing and developed world[41]. Gilbert et al[42] between
1991 and 1996, examined 4121 children in 23 middle-income countries and their
results showed that the prevalence of severe visual impairment or blindness due
to ROP ranged from 0 in most African countries to more than 38% in Cuba.
The
prevalence of ROP has diversity across the countries and states. The existing
data suggest that blindness due ROP varies extremely from country to country, and
globally, over 50 000 children are blind due to ROP[2].
Graziano et al[43] conducted a prospective
examination on 102 neonates with very low BW in Brazil and in their study,
prevalence of ROP was reported 29.09% which is slightly higher than estimated prevalence
in our study (26.1%). Several studies have emphasized that a significant
proportion of blindness due to ROP can be prevented in the presence of a
regular screening program and promote awareness of physicians as well as the
parents[44-45]. Another way to
reduce blindness due to ROP is examination of high-risk newborns in the
neonatal intensive care unit (NICU)[46].
In the present study, after running cumulative Meta-analysis, the
prevalence of ROP showed an increase from 6.0% in 2001 to 24.1% in 2016. This
rise may be explained by improvements in neonatal care in our NICUs, which
leads to increased survival of premature infants. Similar our results, in the
Karkhaneh et al[14] study that performed
in Farabi Hospital as a referral hospital for eyes disease in Iran (the
Tertiary Eye Hospital), a significant increase was observed in the incidence of
ROP. In the Farabi Hospital the incidence of ROP increases from 6% in 1997-1999
to 12.4% in 2000-2002, and 34.5% in 2007[14]. In
the subgroup analysis in our study, the polled estimated prevalence of ROP
before 2010 were 19.2% and after 2010 were increases to 33.9%.
In compare to the prevalence of ROP reported from other countries, ROP
incidence in Iran is higher than some countries. For instance, the incidence of
ROP in infants with GA<31wk or BW<1500 g in France in 2007 was 15%[47] and also the incidence of ROP in infants with BW
<2000 g or GA <34wk was 10.8% in China in 2008[48].
Incidence of ROP in more developed countries was reported between 10% to 27%
and it is depend on degree of prematurity and BW[49-50].
Increase trend in the incidence of ROP represents the better care of the
infants in premature infants in the NICU but on the other hand it should be
keep in mind that these infants needed more attention to problems such as
retinopathy. We conduct a wide search strategy in different databases to
include as many studies as possible. We screened 97 retrieved published papers
and finally included 26 individual studies in the Meta-analysis with 8786
cases. Egger and Begg tests show some evidence of the possibility of
publication bias and in this case we used Trim and Filled method and also
Chi-square and I2 tests show heterogeneity between studies,
therefore we used random effect model in the Meta-analysis and perform
subgroups analysis based on year of publication which is recognized as a
heterogeneity factor in the Meta regression.
In summary, the overall prevalence of ROP is relatively high in
Iran. This disorder can lead to visual impairment or blindness in premature
infants. Much of this burden is avoidable with improved quality of antenatal
and neonatal care, notably oxygen monitoring, and with both screening and
treatment of ROP. Urgent action is required to improve awareness of ROP among
all healthcare professionals involved in the care of premature infants, coupled
with commitments to improve neonatal care, and to develop and implement
protocol and guidelines for the prevention, screening, and treatment of ROP.
ACKNOWLEDGEMENTS
Conflicts of Interest: Maroufizadeh S, None; Almasi-Hashiani A, None; Omani Samani R, None;
Sepidarkish M, None.
REFERENCES
1 Good WV, Hardy RJ, Dobson V, Palmer EA, Phelps DL, Quintos M, Tung B;
Early Treatment for Retinopathy of Prematurity Cooperative Group. The incidence
and course of retinopathy of prematurity: findings from the early treatment for
retinopathy of prematurity study. Pediatrics
2005;116(1):15-23. [CrossRef] [PubMed]
2 Gilbert C, Fielder A, Gordillo L, Quinn G, Semiglia R, Visintin P, Zin
A; International NO-ROP Group. Characteristics of infants with severe
retinopathy of prematurity in countries with low, moderate, and high levels of
development: implications for screening programs. Pediatrics 2005;115(5):518-525. [CrossRef] [PubMed]
3 Darlow BA, Hutchinson JL, Henderson-Smart DJ, Donoghue DA, Simpson JM,
Evans NJ. Prenatal risk factors for severe retinopathy of prematurity among
very preterm infants of the Australian and New Zealand neonatal network. Pediatrics 2005;115(4):990-996. [CrossRef] [PubMed]
4 Kim TI, Sohn J, Pi SY, Yoon YH. Postnatal risk factors of retinopathy
of prematurity. Paediatr Perinat
Epidemiol 2004;18(2):130-134. [CrossRef]
5 Aclimandos W. Seventy years of retinopathy of prematurity. Br J Ophthalmol 2011;95(7):899-900. [CrossRef] [PubMed]
6 Cooke RW, Clark D, Hickey-Dwyer M, Weindling AM. The apparent role of
blood transfusions in the development of retinopathy of prematurity. Eur J Pediatr 1993;152(10):833-836. [CrossRef]
7 Brooks SE, Marcus DM, Gillis D, Pirie E, Johnson MH, Bhatia J. The
effect of blood transfusion protocol on retinopathy of prematurity: a
prospective, randomized study. Pediatrics
1999;104(3):514-518. [CrossRef]
8 Englert JA, Saunders RA, Purohit D, Hulsey TC, Ebeling M. The effect
of anemia on retinopathy of prematurity in extremely low birth weight infants. J Perinatol 2001;21(1): 21-26. [CrossRef] [PubMed]
9 Gupta VP, Dhaliwal U, Sharma R, Gupta P, Rohatgi J. Retinopathy of
prematurity--risk factors. Indian J
Pediatr 2004;71(10):887-892. [CrossRef]
11 Nakshab M, Bayani G,
Ahmadzadeh Amiri A, Eshaghi M. Prevalence of retinopathy in premature neonates
in neonatal intensive care unit of Boali sina hospital in 2001. J Mazandaran Univ Med Sci
2003;13(39): 63-70.
14 Karkhaneh R, Mousavi SZ, Riazi-Esfahani M, Ebrahimzadeh SA, Roohipoor
R, Kadivar M, Ghalichi L, Mohammadi SF, Mansouri MR. Incidence and risk factors
of retinopathy of prematurity in a tertiary eye hospital in Tehran. Br J Ophthalmol 2008;92(11):1446-1449. [CrossRef] [PubMed]
18 Riazi-Esfahani M, Alizadeh Y, Karkhaneh R, Mansouri MR, Kadivar M,
Nili Ahmadabadi M, Nayeri F. Retinopathy of prematurity: single versus
multiple-birth pregnancies. J Ophthalmic
Vis Res 2008;3(1):47-51. [PMC free article] [PubMed]
21 Mousavi SZ, Karkhaneh R, Riazi-Esfahani M, Mansouri MR, Roohipoor R,
Ghalichi L, Kadivar M, Nili-Ahmadabadi M, Naieri F. Retinopathy of prematurity
in infants with late retinal examination. J
Ophthalmic Vis Res 2009;4(1):24-28. [PMC free article] [PubMed]
24 Bayat-Mokhtari M, Pishva N, Attarzadeh A, Hosseini H, Pourarian S.
Incidence and risk factors of retinopathy of prematurity among preterm infants
in Shiraz/Iran. Iran J Pediatr
2010;20(3):303-307. [PMC free article] [PubMed]
27 Ebrahim M, Ahmad RS, Mohammad M. Incidence and risk factors of
retinopathy of prematurity in Babol, North of Iran. Ophthalmic Epidemiol 2010;17(3):166-170. [CrossRef] [PubMed]
28 Ghaseminejad A, Niknafs P. Distribution of retinopathy of prematurity
and its risk factors. Iran J Pediatr
2011;21(2):209-214. [PMC free article] [PubMed]
30 Afarid M, Hosseini H, Abtahi B. Screening for retinopathy of
prematurity in south of Iran. Middle East
Afr J Ophthalmol 2012;19(3):277-281. [CrossRef] [PMC free article] [PubMed]
31 Feghhi M, Altayeb SM, Haghi F, Kasiri A, Farahi F, Dehdashtyan M, Movasaghi
M, Rahim F. Incidence of retinopathy of prematurity and risk factors in the
south-western region of Iran. Middle East
Afr J Ophthalmol 2012;19(1):101-106. [CrossRef] [PMC free article] [PubMed]
32 Abrishami M, Maemori GA, Boskabadi H, Yaeghobi Z, Mafi-Nejad S,
Abrishami M. Incidence and risk factors of retinopathy of prematurity in
Mashhad, Northeast Iran. Iran Red
Crescent Med J 2013;15(3):229-233. [CrossRef] [PMC free article] [PubMed]
33 Sabzehei MK, Afjeh SA, Dastijani Farahani A, Shamshiri AR, Esmaili F.
Retinopathy of prematurity: incidence, risk factors, and outcome. Arch Iran Med 2013;16(9):507-512. [PubMed]
35 Rasoulinejad SA, Montazeri M. Retinopathy of prematurity in neonates
and its risk factors: a seven year study in Northern Iran. Open Ophthalmol J 2016;10 (1):17-21. [CrossRef] [PMC free article] [PubMed]
36 Higgins JP, Thompson SG. Quantifying heterogeneity in a
meta-analysis. Stat Med 2002;21(11):1539-1558.
[CrossRef] [PubMed]
37 Galbraith RF. A note on graphical presentation of estimated odds
ratios from several clinical trials. Stat
Med 1988;7(8):889-894. [CrossRef]
38 Begg CB, Mazumdar M. Operating characteristics of a rank correlation
test for publication bias. Biometrics
1994;50(4):1088-1101. [CrossRef] [PubMed]
39 Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis
detected by a simple, graphical test. BMJ
1997;315(7109):629-634. [CrossRef]
40 Noble JH Jr. Meta-analysis: Methods, strengths, weaknesses, and
political uses. J Lab Clin Med
2006;147(1):7-20. [CrossRef] [PubMed]
41 Chen J, Stahl A, Hellstrom A, Smith LE. Current update on retinopathy
of prematurity: screening and treatment. Curr
Opin Pediatr 2011;23(2): 173-178. [CrossRef] [PMC free article] [PubMed]
42 Gilbert C, Rahi J, Eckstein M, O'Sullivan J, Foster A. Retinopathy of
prematurity in middle-income countries. Lancet
1997;350(9070):12-14. [CrossRef]
43 Graziano RM, Leone CR, Cunha SL, Pinheiro AC. Prevalence of
retinopathy of prematurity in very low birth weight infants. J Pediatr (Rio J) 1997;73(6):377-382. [CrossRef]
44 Modrzejewska M. Retinopathy of prematurity: clinical findings and
current opinions on diagnosis and treatment. Ann Acad Med Stetin 2006;52(1):73-78. [PubMed]
45 Gilbert C. Retinopathy of prematurity: a global perspective of the
epidemics, population of babies at risk and implications for control. Early Hum Dev 2008;84(2):77-82. [CrossRef] [PubMed]
46 Attar MA, Gates MR, Iatrow AM, Lang SW, Bratton SL. Barriers to
screening infants for retinopathy of prematurity after discharge or transfer
from a neonatal intensive care unit. J
Perinatol 2005;25(1):36-40. [CrossRef] [PubMed]
47 Lala-Gitteau E, Majzoub S, Saliba E, Pisella PJ. Epidemiology for
retinopathy of prematurity: risk factors in the Tours hospital (France). J Fr Ophtalmol 2007;30(4):366-373. [CrossRef]
48 Chen Y, Li XX, Yin H, Gilbert C, Liang JH, Jiang YR, Zhao MW; Beijing
ROP Survey Group. Risk factors for retinopathy of prematurity in six neonatal
intensive care units in Beijing, China. Br
J Ophthalmol 2008;92(3):326-330. [CrossRef] [PubMed]
49 Darlow BA, Horwood LJ, Clemett RS. Retinopathy of prematurity: risk
factors in a prospective population-based study. Paediatr Perinat Epidemiol 1992;6(1):62-80. [CrossRef]
50 Early Treatment For Retinopathy Of Prematurity Cooperative Group.
Revised indications for the treatment of retinopathy of prematurity: results of
the early treatment for retinopathy of prematurity randomized trial. Arch Ophthalmol 2003;121(12):1684-1694.
[CrossRef] [PubMed]