
・Clinical
Research・
Clinical
outcomes of transepithelial photorefractive keratectomy versus femtosecond
laser assisted keratomileusis for correction of high myopia in South Egyptian
population
Amr
Mounir1, Engy Mohamed Mostafa1, Hatem Ammar1,
Osama Ali Mohammed1, Alahmady Hamad Alsmman1, Mahmoud
Mohamed Farouk1, Mohamed Gamal Elghobaier2
1Department of Ophthalmology, Sohag
Faculty of Medicine, Sohag University, Sohag 82524, Egypt
2Egyptian Police Hospitals, Cairo
11765, Egypt
Correspondence to: Amr Mounir. Department of
Ophthalmology, Sohag Faculty of Medicine, Sohag University, Sohag 82524, Egypt.
dramrmonir@yahoo.com
Received:
Abstract
AIM: To evaluate the safety
and efficacy of transepithelial photorefractive keratectomy (t-PRK) with
adjuvant mitomycin C (MMC) versus
femtosecond laser assisted keratomileusis
(Femto-LASIK) in correction of high myopia.
METHODS: Prospective randomized
comparative study including 156 eyes of 156 patients with high myopia and a
spherical equivalent refraction (SER) <-6.00 D. They were divided randomly
into two groups: Group A included 72 eyes treated with t-PRK with adjuvant MMC
and Group B included 84 eyes treated with Femto-LASIK. Visual acuity, SER,
corneal topography, pachymetry and keratometry were assessed for 12mo
postoperatively.
RESULTS: The preoperative mean
SER was -8.86±1.81 and -9.25±1.70 D in t-PRK MMC group and Femto-LASIK
respectively (P=0.99) which improved to -0.65±0.43 D and -0.69±0.50 D at
12mo follow up. Mean SER remained stable during the 12mo of follow-up, with no
statistically significant difference between the two groups (P=0.64). In
t-PRK MMC group, only six eyes needed retreatment after six months of follow
up. And two eyes showed haze (one reversible haze grade 2, while the other had
dense irreversible haze grade 4).
CONCLUSION: t-PRK MMC provides
safe and satisfactory visual outcomes and acceptable risk as Femto-LASIK in
patients with high myopia.
KEYWORDS: transepithelial
photorefractive keratectomy; femtosecond laser assisted keratomileusis; high
myopia; corneal haze; Egypt
DOI:10.18240/ijo.2020.01.19
Citation: Mounir
A, Mostafa EM, Ammar H, Mohammed OA, Alsmman AH, Farouk MM, Elghobaier MG.
Clinical outcomes of transepithelial photorefractive keratectomy versus
femtosecond laser assisted keratomileusis for correction of high myopia in
South Egyptian population. Int J Ophthalmol 2020;13(1):129-134
INTRODUCTION
Photorefractive keratectomy (PRK)
was first introduced 30 years ago[1]. Transepithelial
photorefractive keratectomy (t-PRK) was proposed in the late 1990s as an
alternative to conventional PRK. t-PRK removes the epithelium by laser
phototherapeutic keratectomy followed by laser ablation of the stroma[2-3].
Although PRK is an established
procedure for refractive correction of myopia, its popularity was downsized in
favor for laser-assisted in situ keratomileusis (LASIK). Yet PRK is
still needed in conditions where LASIK is not possible. However, postoperative
haze following PRK is not uncommon in eyes undergoing higher degrees of
correction making it the main limiting factor for using laser correction of
vision in this group. Subsequent development of LASIK offered more rapid visual
recovery with less pain and less haze. However, LASIK treatment in eyes with
high myopia results in considerably deeper intrusion into the stroma, with
concerns regarding biomechanical stability and an increased risk of ectasia.
Further, many reports have regarded application of a suction ring during LASIK
to be a potential risk factor for rhegmatogenous retinal detachment, especially
in high myopes, because the procedure might induce vitreous traction and
detachment resulting from sudden decompression of the eye[4-7].
Corneal haze, epithelial healing
abnormalities, and pain are known adverse effects of PRK[8-9]. Development of adjuvant mitomycin C (MMC) therapy as
prophylaxis for haze has demonstrated benefits in the refractive correction of
high myopia and resulted in reappraisal of the role of PRK vs LASIK in
this group[10]. Although postoperative discomfort
is greater and visual recovery is slower compared to LASIK, surface ablation
techniques avoid LASIK flap complications, thus substantially decreasing the
risk of postoperative ectasia[11]. However, there
have been few studies of clinical outcomes of t-PRK in high myopia[12-13] .
The femtosecond laser has been used
in a wide variety of ophthalmological procedures, allowing customization of the
corneal flap parameters, such as diameter, thickness, and hinge position, which
are the main advantages of using the femtosecond laser which lessen the risk of
flap related complications such as buttonholed or incomplete flaps[14-15] .
The aim of this study was to
evaluate the safety and efficacy of t-PRK versus femtosecond laser assisted
keratomileusis (Femto-LASIK) in the correction of high myopia in Egypt. This
region is dry and sunny with high levels of ultraviolet (UV) light, which may
increase the risk of postoperative haze after PRK[16].
SUBJECTS AND METHODS
Ethical Approval The study was approved by the
medical Ethics Committee at the Faculty of Medicine, Sohag University, and
adhered to the Tenets of the Declaration of Helsinki. Written informed consent
was obtained before surgery from all patients. Clinical Trial Registry Number:
PACTR201906529708454.
This prospective comparative
interventional study enrolled patients with high myopia who sought laser vision
correction between April 2016 and May 2017 at Sohag Center for LASIK and
Corneal Surgeries, Sohag, Egypt.
The inclusion criteria were high
myopia [spherical equivalent refraction (SER) <-6.00 D][17].
Age 20-45y, LASIK is not possible for full correction due to thin cornea with
residual stromal bed ≥280 µm[18]. Emmetropia was
the target with full correction of the refractive error. Exclusion criteria
were based on preoperative assessment of ocular topography, and included
corneal dystrophy with topographic irregularity, pellucid marginal
degeneration, forme fruste keratoconus, severe dry eye syndrome, previous
corneal or intraocular surgery, history of current eyelid disease, or any form
of keratitis in addition to patients with a history of keloid formation.
Patients with incomplete 12mo follow up were excluded as well.
The 156 eyes with high myopia were
classified randomly into two groups according to which eye involved right or
left. They were divided randomly into two groups. Group A included 72 eyes
treated with t-PRK with adjuvant MMC and group B included 84 eyes treated with
Femto-LASIK.
All patients were evaluated pre and
postoperatively for the following: manifest uncorrected distant visual acuity
(UCVA), best corrected distant visual acuity (BCVA). Decimal notation was used
to describe the visual acuity, SER, slit-lamp biomicroscopy, intraocular
pressure, and fundus examination. Corneal topography was evaluated using Sirius
Scheimpflug Placido topography (CSO, Florence, Italy).
Preparation for the surgery included
application of prophylactic topical antibiotic eye drops (gatifloxacin 0.3% 5
times per day) in the 24h preoperatively followed by topical anaesthesia
(benoxinate hydrochloride 0.4%) applied 2min before surgery).
After application of povidone iodine
10% surgical scrub on the lashes and eyelids, a closed-loop lid speculum was
applied. In all cases, stromal ablation was carried out by an excimer laser
[VISX S4IR: Abbott Medical Optics (AMO), Santa Ana, CA, USA]. In the t-PRK: 50
µm of epithelium was removed followed by stromal ablation of the exact depth needed.
The stromal bed was washed with cold balanced salt solution[19]
to lessen the thermal effect of laser ablation. After laser ablation, MMC 0.02%
was applied for 40s in all cases.
Femto-LASIK was done after
application of topical anesthesia, a 90-µm thickness flap was created using by
the IntraLase (iFS, Abbott). Femtosecond laser parameters for the corneal flap
creation included bed energy level of 0.85 µJ, a side-cut energy level of 0.95
µJ with superior hinge orientation, flap diameter
A silicone hydrogel bandage contact
lens was applied after laser ablation until complete epithelial healing was
confirmed in t-PRK MMC group. The postoperative medications included topical
antibiotic eye drops (gatifloxacin 0.3% 5 times daily for 1wk), topical steroid
eye drops (prednisolone acetate 1% 5 times daily for 1wk), lubricant eye drops,
and systemic non-steroidal anti-inflammatory drugs. UV protection was advised
and 1000 mg of vitamin C were prescribed for at least 1mo. Gradual tapering of
topical steroids over one month was performed to decrease the risk of corneal
scarring.
Postoperative visits were scheduled
for the first postoperative day, and then at 1wk and 1, 3, 6, and 12mo after
surgery. Each follow-up visit included slit-lamp examination in group A to
detect haze, which was graded according to the method proposed by Fantes et
al[20] as 0 (no haze), 0.5 (trace haze on
oblique illumination), 1 (corneal cloudiness not interfering with visibility of
the fine details of the iris), 2 (mild effacement of the fine details of the
iris), 3 (moderate obscuration of the fine details of the iris), or 4 (details
of the lens and iris not discernible).
Statistical Analysis The data were analyzed using SPSS
for Windows version 18.0 software (SPSS Inc., Chicago, IL, USA). It was used to
compare both groups. A P-value <0.05 was considered to be
statistically significant. Independent sample t-test was used to compare
means of preoperative variables of the 2 groups. Correlation coefficients
including Pearson or Spearman assess the correlation between different
variables under normal conditions.
RESULTS
A total of 156
eyes of 156 patients were enrolled for this prospective study, 60 were males (38.5%) and 96 females
(61.5%). The mean of age of group A was 29.76±5.01y and 27.94±6.69y in group B.
Demographic data for both groups are shown in Table 1. The target refraction in
all patients was emmetropia.
Table 1 Demographic data for both
groups
|
Parameters |
Group A (t-PRK) |
Group B (Femto-LASIK) |
P |
|
Eyes |
72 |
84 |
0.86 |
|
Age (y) |
29.76±5.01 |
27.94±6.69 |
0.731 |
|
Gender (M:F) |
32:40 |
28:56 |
|
In group A, the preoperative mean
SER was -8.86±1.81 D and -9.25±1.70 D in group B with (P=0.99) which
improved to -0.65±0.43 D and -0.69±0.51 D respectively at 12mo follow up (P=0.64;
Figure 1).
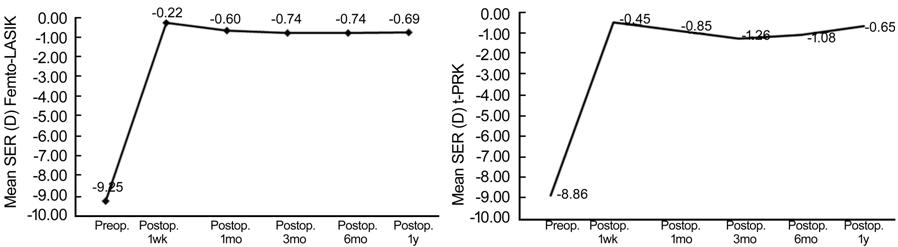
Figure 1 Changes in mean SER in both
groups all over a period of one year follow up.
As regards the visual outcomes; in
group A, the preoperative mean UCVA was 0.05±0.02 and 0.05±
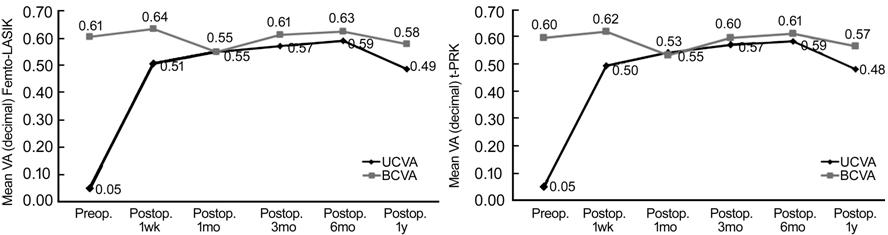
Figure 2 Changes in mean UCVA versus
BCVA in both groups all over a period of one year follow up.
Twelve-month changes in vision and
refraction indices between the two groups are compared in Table 2, comparison
of baseline parameters showed no significant difference between the two groups
preoperatively (all P>0.05).
Table 2 Twelve-month changes in
vision and refraction indices between the two groups
|
Parameters |
Preop. |
P |
1wk |
P |
1mo |
P |
3mo |
P |
6mo |
P |
1y |
P |
|
|
UCVA |
Femto |
0.05±0.01 |
0.96 |
0.51±0.17 |
0.47 |
0.55±0.17 |
0.49 |
0.57±0.18 |
0.57 |
0.59±0.17 |
0.48 |
0.49±0.18 |
0.53 |
|
t-PRK |
0.05±0.02 |
0.50±0.15 |
0.54±0.16 |
0.56±0.17 |
0.58±0.16 |
0.48±0.17 |
|||||||
|
BCVA |
Femto |
0.61±0.17 |
0.47 |
0.64±0.17 |
0.41 |
0.55±0.18 |
0.51 |
0.61±0.16 |
0.41 |
0.63±0.16 |
0.45 |
0.58±0.17 |
0.45 |
|
t-PRK |
0.60±0.15 |
0.63±0.15 |
0.54±0.16 |
0.60±0.15 |
0.62±0.15 |
0.57±0.15 |
|||||||
|
SER |
Femto |
-9.25±1.70 |
0.99 |
-0.22±0.67 |
0.2 |
-0.60±0.59 |
0.005 |
-0.74±0.49 |
0.01 |
-0.74±0.48 |
0.001 |
-0.69±0.51 |
0.64 |
|
t-PRK |
-8.86±1.81 |
-0.45±0.98 |
-0.85±0.95 |
-1.26±0.96 |
-1.08±0.92 |
-0.65±0.43 |
|||||||
|
Sphere |
Femto |
-7.88 |
0.79 |
-0.15 |
0.23 |
-0.39 |
0.004 |
-0.49 |
0.001 |
-0.55 |
0.001 |
-0.46 |
0.156 |
|
t-PRK |
-7.50 |
-0.36 |
-0.64 |
-1.01 |
-0.88 |
-0.45 |
|||||||
|
Cylinder |
Femto |
-2.73 |
0.01 |
-0.14 |
0.51 |
-0.42 |
0.27 |
-0.50 |
0.30 |
-0.39 |
0.20 |
-0.48 |
0.07 |
|
t-PRK |
-2.72 |
-0.18 |
-0.42 |
-0.50 |
-0.40 |
-0.41 |
|||||||
P-value for comparison of
postoperative value all over 12mo of follow-up with the preoperative value;
UCVA: Uncorrected distant visual acuity; BCVA: Best corrected distant visual
acuity; SER: Spherical equivalent refraction.
Scattergram of attempted versus
achieved mean SER for Femto-LASIK group and t-PRK at 12mo postoperatively was
shown in Figure 3.
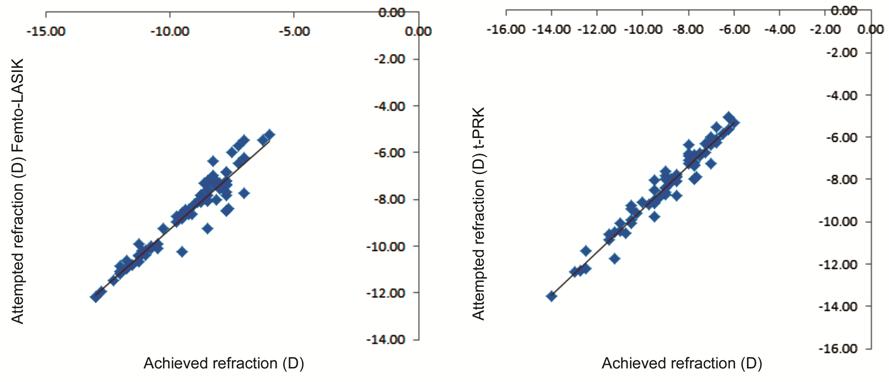
Figure 3 Scattergram of attempted
versus achieved mean SER for both groups at 12mo postoperatively.
The safety indices (ratio of the
mean BCVA at 12mo postoperatively to the mean preoperative BCVA), the efficacy
indices (the ratio of the mean postoperative UCVA to the mean preoperative BCVA
at 12mo) and predictability of both groups were summarized in Table 3.
Table 3 Safety, efficacy and
predictability of both groups at 12mo
|
Parameters |
Group A (t-PRK) |
Group B (Femto-LASIK) |
|
Safety (%) |
95.0 |
95.1 |
|
Efficacy (%) |
80.0 |
80.3 |
|
Predictability (%) |
|
|
|
SER within 1.00 (D) |
71.43 |
85.71 |
|
SER within 1.50 (D) |
84.52 |
95.24 |
Regarding stability at 12mo
postoperatively, both procedures were stable with no statistically significant
differences among the measured SER.
Six eyes needed retreatment due to
marked regression <-1.00 D at six months of follow up. After patient
consultation with the surgeon and checking the availability of enough corneal
thickness, another t-PRK retreatment was done to reach the desired refraction.
Patients were satisfied with UCVA of 0.3±0.10 at the end of the 12mo follow up
period.
Five eyes in the study population
developed complications, comprising delayed epithelial healing in two eyes and
complete healing occurred only after cessation of topical steroids. Corneal
haze developed in two eyes of two patients (one eye with grade 2 haze at 3mo
that improved with topical steroids and the other eye with dense irreversible
grade 4 haze at 2mo and necessitated lamellar keratoplasty). One eye suffered
from toxic epitheliopathy (an unhealthy thickened irregular epithelial surface
with punctate epithelial erosions and opacification extending from the
epithelial surface down to the subepithelial and superficial stromal regions)
which was controlled by switch from preserved to preservative-free eye drops
with UCVA of 0.3±0.12 at the end of the 12mo follow up period (Figure 4).
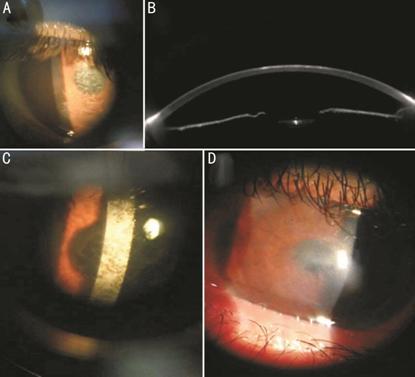
Figure 4 Postoperative complications
of t-PRK in the studied population A: Haze grade 2; B: Scheimpflug
imaging of the same eye; C: Haze grade 4; D: Toxic epitheliopathy.
Complications in the Femto-LASIK
group included two eyes with released suction ring and two eyes with
microstriae which were corrected by re-floating the flap.
DISCUSSION
PRK is a safe and effective
technique for correction of low and moderate myopia[19].
However, its clinical outcomes in highly myopic eyes need to be evaluated in
more detail especially in dry and sunny environments. High levels of UV
exposure may increase the risk of corneal haze.
In our study, epithelium was removed
using the excimer laser which we preferred due to the homogeneous and uniform
epithelial removal. Epithelial removal using laser has superior impact on
postoperative pain and on subepithelial opacification[21-22].
In a study that compared the visual
outcomes and safety of t-PRK and conventional PRK in eyes with low to moderate
myopia, Naderi et al[2] found that t-PRK
was superior to conventional PRK in terms of improving safety and efficacy
indices and visual acuity. Our findings showed significant improvement in UCVA
(P<0.0001) with a high safety index (0.95). This is particularly
significant because our subjects were high myopes in a high UV environment and
were followed for at least 1y.
Our results agreed with those of
Adib-Moghaddam et al[23] who reported a
high degree of safety and visual improvement after t-PRK in patients with
myopia up to -8.75 D during 18mo of follow-up.
In the current study, postoperative
refraction was stable, with no statistically significant regression observed
recorded during 12mo of follow-up. This finding is in agreement with that of
Kaluzny et al[13] who compared t-PRK and
alcohol-assisted PRK in eyes with moderate myopia and compound myopic
astigmatism correction and reported that the mean refractive spherical
equivalent was stable during 3mo of follow-up.
However, not all studies coincide
with our results. A study by Buratto et al[24],
found that 29 of 40 eyes treated by PRK showed regression of myopia by 6mo
after surgery.
Our results confirm that the use of
MMC in a concentration of 0.02% for 40s yielded better visual results and less
haze which was most feared. The efficacy of MMC was investigated in different
studies with different concentrations and different application time[25-28].
The predictability of t-PRK group
demonstrates good refractive predictability at 1y (84.52%) but less than
Femto-LASIK group. These results are consistent with those of Dausch et al[29] who investigated the clinical outcomes of PRK for
myopia exceeding -8.00 D using a standard or aspherical optimized profile in
100 eyes and demonstrated high predictability for both techniques over a
follow-up duration of 1y.
Also, in a study of Hashemi et al[30] who compared the results of Femto-LASIK and PRK
with MMC for the correction of myopia more than 7.0 D, they found that
differences between both groups in baseline indices were not statistically
significant at 6mo after surgery which coincides with our results.
Hashmani et al[31] studied visual outcomes and satisfaction among
patients of PRK and femtosecond LASIK. They found the efficacy indexes of the
femto-Lasik and PRK groups were 1.00 and 0.82, respectively. The predictability
of the procedures was 92.1% and 64.9% which is lower than our results.
The low incidence of haze in our
study can be explained by application of MMC 0.02% for 40s, as in a study by
Kremer et al[32] who reported a decreased
risk of haze following PRK with application of MMC in 1520 eyes, even in eyes
with delayed epithelial healing.
Cooling the corneal bed with cold
balanced salt solution as a routine step in our excimer laser treatment is also
beneficial because it lessens the thermal effect of laser ablation, which in
turn decreases formation of corneal haze. The beneficial effect of this
technique was seen in a study by Niizuma et al[19]
who investigated the ability of cold balanced salt solution to reduce the risk
of subepithelial haze. Stein et al[33]
also investigated the effect of cooling the cornea during PRK to reduce
postoperative corneal haze and found that haze was significantly reduced in
eyes that were irrigated with cold balanced salt solution.
In conclusion, the results of t-PRK
in patients with high myopia in Egypt with hot sunny weather is was shown to be
safe with high efficacy in decreasing refractive error and acceptable risk through
1y of follow-up. Further studies are warranted to investigate if similar
techniques can produce acceptable results in extreme myopia (SE<-10.00).
ACKNOWLEDGEMENTS
Conflicts of Interest: Mounir A, None; Mostafa
EM, None; Ammar H, None; Mohammed OA, None; Alsmman AH,
None; Farouk MM, None; Elghobaier MG, None.
REFERENCES
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||