
・Letter
to the Editor・
Ultrasound
cyclo plasty for the management of glaucoma secondary to ocular irradiation for
choroidal melanoma
Stefano Sebastiani1,2, Mónica Asencio-Durán3, Cosme Lavín-Dapena3, Beatriz Manzano-Muñoz3, Oriana D’Anna-Mardero3, Rosa Cordero-Ros3,
Marco Pellegrini1, Federico Bernabei1, Andrea Mercanti2,
Vincenzo Scorcia4, Giuseppe Giannaccare1,4
1Ophthalmology
Unit, S. Orsola-Malpighi Hospital, University of Bologna, Bologna 40138, Italy
2Ophthalmology
Unit, Infermi Hospital, Rimini 47838, Italy
3Ophthalmology
Department, Hospital Universitario La Paz, Madrid 28046, Spain
4Department of
Ophthalmology, University of “Magna Graecia”, Catanzaro 88100, Italy
Correspondence
to: Giuseppe Giannaccare. Department of Ophthalmology, University of “Magna
Graecia”, Catanzaro 88100, Italy. giuseppe.giannaccare@gmail.com
Received:
DOI:10.18240/ijo.2020.01.26
Citation: Sebastiani S, Asencio-Durán M,
Lavín-Dapena C, Manzano-Muñoz B, D’Anna-Mardero O, Cordero-Ros R, Pellegrini M,
Bernabei F, Mercanti A, Scorcia V, Giannaccare G. Ultrasound cyclo plasty for
the management of glaucoma secondary to ocular irradiation for choroidal
melanoma. Int J Ophthalmol 2020;13(1):184-188
Dear Editor,
In the past, enucleation has been
considered the only available option and the standard of care for the
management of malignant intraocular tumors. Thanks to the advances in the field
of radiotherapy, new therapeutic approaches have been developed in the last decades,
such as plaque brachytherapy and proton beam therapy (PBT)[1]. These
techniques allow to preserve the eyeball and obtain local control of the tumor,
maintaining a certain visual function in an increasingly higher proportion of
cases, without any difference in terms of survival and metastasis-free outcomes
compared to enucleation[1].
However, sight- and
eyeball-threatening complications including neovascular glaucoma (NVG),
radiation retinopathy and optic neuropathy can complicate the postoperative
course of ocular irradiation, with detrimental effects on patients’ vision and
quality of life[1-4]. In particular, NVG occurs in up to 27% of
these cases[1], and represents one of the most common causes of
secondary enucleation[5]. In fact, despite maximum anti-glaucoma
medications, intraocular pressure (IOP) is often not well controlled in this
setting. In addition, European Glaucoma Society (EGS) guidelines discourage the
use of prostaglandin analogues and pilocarpine due to the theoretical risk of
promoting metastasis dissemination[6]. A further issue is related to
patients’ intolerance to active agents and preservatives of anti-glaucoma
medications, which can worsen dry eye disease and corneal/conjunctival
epitheliopathy secondary to anterior segment irradiation. Finally, EGS
guidelines as well as other authors suggest also that incisional glaucoma
surgery is indicated only after successful irradiation therapy with local tumor
control to prevent extraocular tumor extension due to the possible risks of
inoculation metastasis and local recurrence[7-9].
Taking into account all these
factors, the management of glaucoma secondary to ocular irradiation for
choroidal melanoma represents a real therapeutic challenge for ophthalmologist.
We report herein the feasibility and
the outcomes of ultrasound cyclo plasty (UCP) performed as first-line surgical
treatment in 3 eyes of 3 patients with glaucoma secondary to ocular irradiation
(PBT and brachytherapy) for the treatment of choroidal melanoma.
UCP device (EyeOP1, Eye Tech Care,
Rillieux-la-Pape, France) uses high-intensity focused ultrasound (HIFU) to
achieve a selective and more precise coagulation of the ciliary body, while
sparing the adjacent ocular structures. The procedure has been previously
described in details by our group[10]. Briefly, the device is
composed by a coupling cone and a ring probe containing 6 piezoelectric
transducers. The 6 transducers produce and deliver HIFU beams operating at a
frequency of 21 MHz with an acoustic power of 2 W, being able to determine the
fast increase of ciliary body temperature up to
Written informed consent was
obtained from all the subjects included in this case series before any
procedure. This case series was conducted in accordance with the tenets of the
Declaration of Helsinki and was approved by the local Institutional Review
Board.
CASE 1
A 44 year-old woman was referred to
the Retina Service of S. Orsola-Malpighi University Hospital (Bologna, Italy)
for a mushroom-shaped choroidal melanoma of
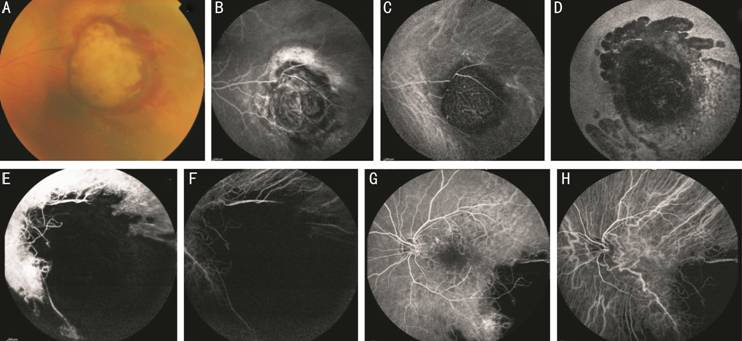
Figure 1 Case 1 Fundus photography (A),
fluorescein angiography (B) and indocyanine green angiography (C) showing the
mushroom-shaped choroidal melanoma. Note the characteristic “double
circulation” pattern of the choroidal melanoma consisting of normal retinal
vessels overlying the internal circulation within the lesion. Fundus
autofluorescence (D), fluorescein angiography (E) and indocyanine green
angiography (F) showing the lesion 1y after PBT with atrophy of the surrounding
retina and choroid. Fluorescein angiography (G) and indocyanine green
angiography (H) showing radiation retinopathy involving the macular region,
capillary leakage and retinal capillary dropout with foveal avascular zone
enlargement.
One year after irradiation
treatment, patient came to our attention complaining of decreased visual acuity
(20/50) in the treated eye. Slit lamp examination showed iris
neovascularization in about 3 clock hours and IOP was found to be
Topical anti-glaucoma therapy was
initiated with fixed combination dorzolamide-timolol eye drop twice daily and
brimonidine eye drop twice daily. In the following months, the further addition
of oral carbonic anhydrase inhibitor (CAI) tablets (250 mg, 1 tablet twice
daily) was necessary to better control IOP values. Two years after PBT, best
corrected visual acuity was stable at 20/50, while IOP was found again high (
One day postoperatively, IOP was
reduced to
During the following scheduled visits,
IOP was approximately stable (values of 15, 18 and
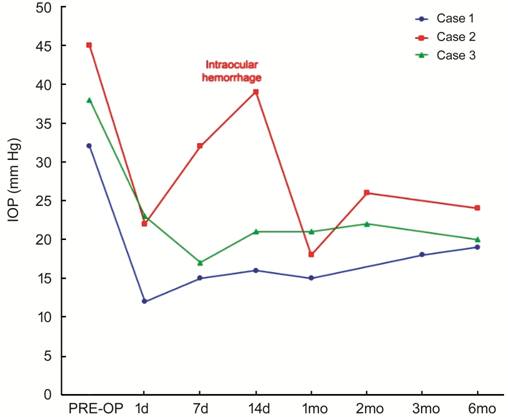
Figure 2 IOP changes of the treated
patients during the 6-months follow-up period The IOP spike in Case 2 was found when
intraocular hemorrhage occurred, with subsequent spontaneous resolution and IOP
reduction.
CASE 2
A 76 years-old woman was treated at
the Retina Service of Hospital La Paz (Madrid, Spain) with I-125 brachytherapy
for a choroidal melanoma of
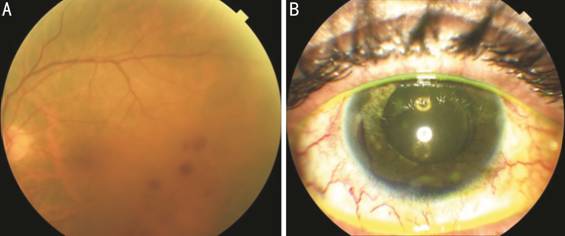
Figure 3 Case 2 Fundus photography (A) showing radiation
retinopathy with scattered dot and blot retinal hemorrhages in the temporal
macular region. Anterior segment photography (B) showing the hyphema occurred
1wk after UCP procedure.
The postoperative course was stable
until the 8-year post-brachytherapy visit, when best corrected visual acuity
was 20/200 and IOP was
CASE 3
A 58 years-old man was diagnosed
with a large choroidal melanoma of
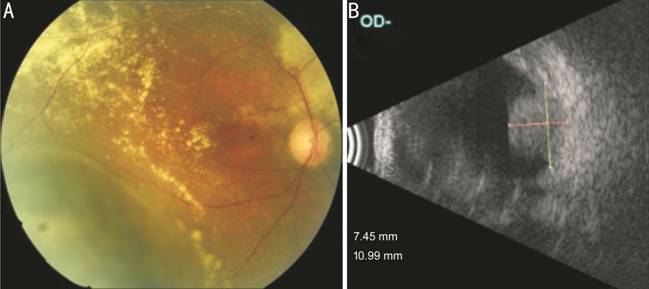
Figure 4 Case 3 Fundus photography (A) showing the
choroidal melanoma in the inferotemporal region with surrounding retinal
exudation. B-scan ultrasonography (B) showing the solid hyperechoic choroidal
mass protruding in the vitreous chamber.
In the attempt of reducing IOP and
controlling eye pain, UCP treatment was performed in the right eye. One day
postoperatively, IOP dropped to
Intraocular tumors can cause
secondary glaucoma through different ways such as solid tumor invasion and
tumor seeding into the angle, angle closure, and iris neovascularization[9].
However, secondary glaucoma can often complicate the postoperative course after
ocular irradiation treatments[8].
UCP uses HIFU beams to induce a
precise, well-controlled and selective tissue coagulation of the ciliary body,
while sparing adjacent ocular structures[12-13]. This non-incisional
minimally-invasive procedure allows for a more predictable and controlled IOP
reduction, with lower complications rates and better preservation of visual
acuity compared to traditional cyclodestructive techniques. In fact, the latter
are currently generally indicated for eyes with refractory or end-stage
glaucoma and poor visual potential, due to their non-selectivity and
unpredictable dose-effect relationship, with the risk of severe complications
as chronic hypotony, vision loss and phthisis[14].
In previous studies, UCP procedure
showed to be safe and effective, reducing both IOP values and hypotensive
medications, without detrimental effects on visual function[10,12-13,15-17].
To date, UCP has been used with a
good profile of safety and efficacy in different stages and types of glaucoma,
such as primary open angle, chronic angle closure, pseudoexfoliative, uveitic,
neovascular and others[12-13,15-17]. To the best of our knowledge,
no previous reports of glaucoma secondary to ocular irradiation for choroidal
melanoma treated with UCP have been described to date.
Nowadays, the progresses in ocular
radiotherapy allow preserving a certain visual function in an ever-increasing
number of cases, even after highly invasive treatments. In the attempt of being
less invasive and trying to preserve patients’ residual visual function, we
performed UCP that is a more conservative treatment with lower complications
rates compared to traditional cyclodestructive techniques. The other additional
advantage over conventional incisional surgical techniques (e.g.,
trabeculectomy, shunt implantation) is the presumed lower risk of inoculation
metastasis and local recurrence, as stated by EGS guidelines and other authors[6,8-9].
In all cases, UCP showed a good hypotensive effect, with an IOP reduction of
about 40% 6mo after the procedure, allowing at the same time the reduction of
the daily number of topical and oral hypotensive medications used. Since the
UCP procedure is “conjunctival-sparing”, it is indicated also in eyes with
chronic conjunctival inflammation and fibrotic or necrotic tissues alterations
affecting wound healing, as can occur after ocular proton beam irradiation or
in multi-operated eyes.
The main limitation of the study is
the limited follow-up of 6mo. In fact, like for other cyclodestructive
procedures, the efficacy of UCP may be partial or time-limited, mainly due to
the possible re-epithelialization process of the ciliary processes with progressive
recovery of their function[18]. However, repeated treatments are
possible in case of qualified success in order to enhance efficacy and further
reduce IOP without any detrimental effect, as previously described[17].
In conclusion, UCP might add a new additional
step between medical and surgical therapeutic options for challenging cases of
glaucoma, like those presented in this case series, thus providing a new
minimally invasive option to be added in the current armamentarium of glaucoma
treatments.
ACKNOWLEDGEMENTS
Conflicts of Interest: Sebastiani S, None; Asencio-Durán
M, None; Lavín-Dapena C, None; Manzano-Muñoz B, None; D’Anna-Mardero O,
None; Cordero-Ros R, None; Pellegrini M, None; Bernabei F,
None; Mercanti A, None; Scorcia V, None; Giannaccare G,
None.
REFERENCES
|
1 Bensoussan E, Thariat J, Maschi C, Delas J, Schouver
ED, Hérault J, Baillif S, Caujolle JP. Outcomes after proton beam therapy for
large choroidal melanomas in 492 patients. Am J Ophthalmol 2016;165:78-87. |
|
|
|
|
|
2 Floriani I, Quaranta L, Rulli E, Katsanos A, Varano
L, Frezzotti P, Rossi GC, Carmassi L, Rolle T, Ratiglia R, Gandolfi S,
Fossarello M, Uva M, Hollander L, Poli D, Grignolo F, Italian Study Group on
QoL in glaucoma. Health-related quality of life in patients with primary
open-angle glaucoma. An Italian multicentre observational study. Acta
Ophthalmol 2016;94(5):e278-e286. |
|
|
|
|
|
3 Rulli E, Quaranta L, Riva I, Poli D, Hollander L,
Galli F, Katsanos A, Oddone F, Torri V, Weinreb RN, Italian Study Group on
QoL in Glaucoma. Visual field loss and vision-related quality of life in the
Italian primary open angle glaucoma study. Sci Rep 2018;8(1):619. |
|
|
|
|
|
4 Riva I, Legramandi L, Katsanos A, Oddone F, Rulli E,
Roberti G, Quaranta L; Italian Study Group on QoL in Glaucoma. Influence of
sociodemographic factors on disease characteristics and vision-related
quality of life in primary open-angle glaucoma patients: the Italian primary
open angle glaucoma study (IPOAGS). J Glaucoma 2018;27(9):776-784. |
|
|
|
|
|
5 Fabian ID, Tomkins-Netzer O, Stoker I, Arora AK,
Sagoo MS, Cohen VM. Secondary enucleations for uveal melanoma: a 7-year
retrospective analysis. Am J Ophthalmol 2015;160(6):1104-1110.e1. |
|
|
|
|
|
6 European glaucoma society terminology and guidelines
for glaucoma, 4th edition-Chapter 2: classification and terminologysupported
by the EGS foundation. Br J Ophthalmol 2017;101(5):73-127. |
|
|
|
|
|
7 Conway RM, Poothullil AM, Daftari IK, Weinberg V,
Chung JE, O'Brien JM. Estimates of ocular and visual retention following
treatment of extra-large uveal melanomas by proton beam radiotherapy. Arch
Ophthalmol 2006;124(6):838-843. |
|
|
|
|
|
8 Riechardt AI, Cordini D, Rehak M, Hager A, Seibel I,
Böker A, Gundlach E, Heufelder J, Joussen AM. Trabeculectomy in patients with
uveal melanoma after proton beam therapy. Graefes Arch Clin Exp Ophthalmol
2016;254(7):1379-1385. |
|
|
|
|
|
9 Camp DA, Yadav P, Dalvin LA, Shields CL. Glaucoma
secondary to intraocular tumors: mechanisms and management. Curr Opin
Ophthalmol 2019;30(2):71-81. |
|
|
|
|
|
10 Giannaccare G, Sebastiani S, Campos EC. Ultrasound
cyclo plasty in eyes with glaucoma. J Vis Exp 2018(131). |
|
|
|
|
|
11 Egger E, Schalenbourg A, Zografos L, Bercher L,
Boehringer T, Chamot L, Goitein G. Maximizing local tumor control and
survival after proton beam radiotherapy of uveal melanoma. Int J Radiat Oncol
Biol Phys 2001;51(1):138-147. |
|
|
|
|
|
12 Denis P, Aptel F, Rouland JF, Nordmann JP, Lachkar
Y, Renard JP, Sellem E, Baudouin C, Bron A. Cyclocoagulation of the ciliary
bodies by high-intensity focused ultrasound: a 12-month multicenter study.
Invest Ophthalmol Vis Sci 2015;56(2):1089-1096. |
|
|
|
|
|
13. Aptel F, Denis P, Rouland JF, Renard JP, Bron A.
Multicenter clinical trial of high-intensity focused ultrasound treatment in
glaucoma patients without previous filtering surgery. Acta Ophthalmol
2016;94(5):e268-e277. |
|
|
|
|
|
14 Iliev ME, Gerber S. Long-term outcome of
trans-scleral diode laser cyclophotocoagulation in refractory glaucoma. Br J
Ophthalmol 2007;91(12):1631-1635. |
|
|
|
|
|
15 Giannaccare G, Vagge A, Gizzi C, Bagnis A,
Sebastiani S, Del Noce C, Fresina M, Traverso CE, Campos EC. High-intensity
focused ultrasound treatment in patients with refractory glaucoma. Graefes
Arch Clin Exp Ophthalmol 2017;255(3):599-605. |
|
|
|
|
|
16 Giannaccare G, Vagge A, Sebastiani S, Urbini LE,
Corazza P, Pellegrini M, Carmassi L, Bergamini F, Traverso CE, Campos EC.
Ultrasound cyclo-plasty in patients with glaucoma: 1-year results from a
multicentre prospective study. Ophthalmic Res 2019;61(3):137-142. |
|
|
|
|
|
17 Pellegrini M, Sebastiani S, Giannaccare G, Campos
EC. Intraocular inflammation after ultrasound cyclo plasty for the treatment
of glaucoma. Int J Ophthalmol 2019;12(2):338-341. |
|
|
|
|
|
18 McKelvie PA, Walland MJ. Pathology of cyclodiode
laser: a series of nine enucleated eyes. Br J Ophthalmol 2002;86(4):381-386. |
|