IF in JCR CiteScore
Rank About IJO Current
Issue Featured Articles Articles In Press Recent Accepted
 International Journal
of Ophthalmology
International Journal
of Ophthalmology
2017; 10(9): 1452-1459
・Investigation・
Predictive factors of visual outcome of Malaysian
cataract patients: a retrospective study
Thanigasalam Thevi1, Myron Anthony
Godinho2
1Department
of Ophthalmology, Melaka Hospital, Jalan Mufti Haji Khalil, Melaka 75400,
Malaysia
2Public
Health Evidence South Asia, Manipal University, Manipal 576104, India
Correspondence
to: Thanigasalam Thevi. Department of Ophthalmology, Melaka Hospital,
Jalan Mufti Haji Khalil, Melaka 75400, Malaysia.111thevi@gmail.com
Received:
2016-10-19
Accepted: 2017-03-31
Abstract
AIM: To explore the associations between
various characteristics of Malaysian cataract patients and their management,
and their post-operative visual outcomes, to inform relevant bodies to reduce
cataract-related blindness.
METHODS: We conducted a descriptive
secondary data analysis of cataract surgery patients in Melaka Hospital, from
2007 to 2014 using the National Eye Database (NED). Patient-related factors
(demographic features, systemic and ocular comorbidities) and management-related
factors (surgical duration, type of surgery, type of lens) were analysed for
their association with visual outcome (acuity).
RESULTS: Most patients were Malays (48.23%)
and Chinese (38.55%) aged 60-79y (range 0-100y). Hypertension (58.61%) and diabetes
(44.89%) were major systemic comorbidities. Glaucoma (6.71%) and diabetic
retinopathy (10.12%) were the main ocular comorbidities. Other comorbidities
were age-related macular degeneration, pterygium, corneal opacities, macula
diseases, vitreous haemorrhage, retinal detachment and pseudoexfoliation
(0.70%-1.60%). Preoperatively 7150 (55.03%) eyes presented with poor vision.
Uncomplicated phacoemulsification performed quickly with foldable lenses gave
good results.
CONCLUSION: Primary care physicians should
initiate early detection to prevent late presentation of cataracts causing poor
vision and should discuss the risks and benefits of cataract surgery while
emphasizing the role of pre-existing comorbidities which may affect the visual
outcomes. For good results, phacoemulsification should be done within 30min,
without complications, using foldable posterior chamber intraocular lens.
KEYWORDS: cataract;
presenting features; predictors; visual outcome
Citation: Thevi T, Godinho MA. Predictive factors of visual outcome of Malaysian
cataract patients: a retrospective study. Int J Ophthalmol 2017;10(9):
1452-1459
INTRODUCTION
The
Malaysian National Eye Survey reported that cataracts were the leading cause of
blindness (39%) and poor vision (36%) in Malaysia[1].
The decision to undergo cataract surgery should be facilitated by an informed,
evidence-based, preoperative discussion between doctor and patient, addressing
the various reasons to undergo or avoid surgery. Estimates of visual prognosis
should aid in decision-making, and patients should be counseled on the risks
and outcomes, should complications arise. Differences in visual outcome should
be explained, as realistic patient expectations may reduce the risk of medicolegal litigation too[2].
As cataracts are most commonly due to aging, patients present with a
number of age-related ocular and systemic diseases which pose challenges in patient
management. For example, diabetics are suspected to have an increased risk of Streptococcus-related
post-operative endophthalmitis[3]. Systemic
hypertension too has been associated with intraoperative complications such as
suprachoroidal haemorrhage, although recent evidence questions this[4]. Despite
universal healthcare provision in Malaysia, poor attendance at regular health
screening results in undiagnosed cases of diabetes and hypertension. A
community-based study at a French National Eye Centre suggested that up to 14%
of presenting patients may have undiagnosed diabetes mellitus (DM)[5]. Often,
deranged parameters are discovered only at the pre-operative assessment, and
control of these can require hospitalisation and month-long delays in treatment.
This negates the main benefits of day-care surgery, like cost-reduction and
same-day discharge. Ideally, blood pressure and blood sugar levels should be
controlled through early detection and treatment by the primary care doctor
(family physician or general practitioner) prior to an ophthalmology referral.
Another issue is the number of late-presenters. Malaysian patients still
present with cataracts causing poor visual acuities bilaterally. These patients
often have mature/hypermature cataracts and require urgent surgical treatment,
resulting in postponement of treatment for patients who are already waitlisted.
This phenomenon can also be prevented by early detection and referral.
This study aims to assess the factors determining the visual outcome of
cataract surgery, and discuss how these can inform an evidence-based
pre-operative discussion between doctor and patient, to provide better patient
education, ensure realistic patient expectations, and avoid unnecessary
surgeries in high-risk patients.
SUBJECTS AND METHODS
We conducted an 8-year (2007-2014) retrospective analysis of secondary
data using the National Eye Database (NED) of Melaka Hospital of patients who
underwent cataract surgeries in Melaka Hospital. Approval was granted by
Medical Research Ethics Committee of Malaysia. Melaka Hospital is an 806-bed
government-funded specialist public hospital serving as a referral centre for
Melaka State, the northern parts of Johor State and the Tampin District of
Negeri Sembilan State[6].
We studied the relationship between patients’ demographic features (e.g.
age groups, ethnicities etc.), procedural features and complications;
and their final outcome (visual acuity). We classified the patients by age
groups into less than 40y, 41-60y, 61-80y and above 80y. Ethnicity was
classified as Malay, Chinese and Indian which comprised of the 3 main races of
the country. Others included Eurasian, Portuguese, Sri Lankan and foreign
nationals such as Nepalese, Vietnamese, Myanmar, Cambodians, Bangladeshis and
Indonesians. We classified visual acuity as ‘good’ (logMAR 0.0 to 0.3),
‘impaired’ (logMAR 0.50 to 0.80) or ‘poor’ [logMAR 1.00, hand movement (HM),
light perception (LP) and no light perception (NLP)]. Visual
outcome was recorded as the best corrected visual acuity, based on refractions
performed by hospital-based optometrists, recorded at 12wk postoperatively.
We noted the cataract aetiology as either primary
(congenital/developmental/senile) or secondary
(drug-induced/traumatic/surgical). Chronic multi-system diseases were grouped
as ‘systemic comorbidities’. Diseases with chronic local effects limited to the
eyeball and orbit were grouped as ‘ocular comorbidities’. We also noted
management-related factors and their association with the final visual outcome.
We
recorded the types of cataract surgeries and duration, and analyzed to
determine their associations with visual outcomes. Whether cataract surgery was
done alone or in combination with other ocular surgeries was also studied for
its effect on visual outcome. The cumulative prevalence of intra-operative
complications and post-operative complications were recorded and their
associations with visual outcome were studied. We looked at associations of
types of intraocular lenses (IOLs) and outcomes.
Odds ratios (OR), confidence interval and P values were
calculated for each of the 3 visual acuity classes, compared to the rest of the
patient population. Data analysis was performed using Epi-info 7 (freeware).
RESULTS
Some data were missing from the database and hence, we analysed only
available data in various sections of the results. Figure 1 shows the age
distribution of patients who underwent cataract surgery at Melaka Hospital from
2007-2014. As shown, cataracts can occur at any age, but tend to be among the
elderly, normally distributed around a mean of 65 with a standard deviation of
11.09. The box-plot illustrates a median of 66, with an equally distributed
interquartile range of 12 (60 to 72). The age-grouped bar chart eliminates
tails: over 70% of patients are aged between 61 and 80. Table 1 shows that
those aged less than 40y and over 80y were at greater risk of a poor visual
outcome, with OR of 3.74 and 1.51 respectively.
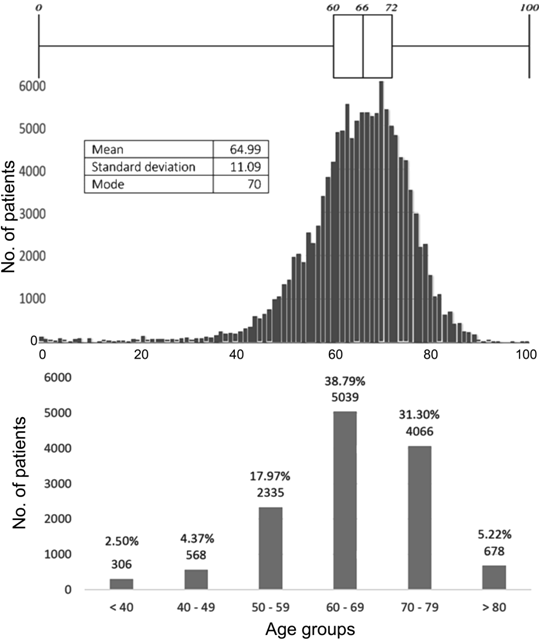
Figure 1 Age distribution of cataract surgery patients at Melaka
Hospital, 2007-2014.
Table 1 Association between visual outcome and various patient-related
factors and procedure-related factors
|
Visual outcome |
Total |
% |
Good visual outcome |
Impaired visual outcome |
Poor visual outcome |
||||||
|
OR |
95%CI |
P |
OR |
95%CI |
P |
OR |
95%CI |
P |
|||
|
Age grouping (a) |
|
|
|
|
|
|
|
|
|
|
|
|
<40 |
325 |
2.50 |
0.34 |
(026-0.43) |
<0.01 |
1.71 |
(1.28-2.27) |
<0.01 |
3.74 |
(1.79-5.00) |
<0.01 |
|
41-60 |
2884 |
22.20 |
1.06 |
(0.96-1.17) |
0.27 |
0.78 |
(0.69-0.88) |
<0.01 |
1.32 |
(1.13-1.53) |
<0.01 |
|
61-80 |
9105 |
70.08 |
1.36 |
(1.25-1.49) |
<0.01 |
0.90 |
(0.1-1.00) |
0.04 |
0.58 |
(0.50-0.66) |
<0.01 |
|
>80 |
678 |
5.22 |
0.45 |
(0.38-0.53) |
<0.01 |
2.25 |
(1.87-2.71) |
<0.01 |
1.51 |
(1.15-1.97) |
<0.01 |
|
Race |
|
|
|
|
|
|
|
|
|
|
|
|
Malay |
6209 |
47.79 |
0.89 |
(0.82-0.97) |
<0.01 |
0.98 |
(0.89-1.09) |
0.73 |
1.37 |
(1.20-1.57) |
<0.01 |
|
Chinese |
4963 |
38.20 |
1.10 |
(1.01-1.20) |
0.03 |
1.01 |
(0.91-1.12) |
0.88 |
0.77 |
(0.67-0.89) |
<0.01 |
|
Indian |
1608 |
12.37 |
1.07 |
(0.94-1.23) |
0.28 |
1.00 |
(0.86-1.16) |
0.99 |
0.83 |
(0.67-1.03) |
0.08 |
|
Other |
93 |
0.72 |
0.78 |
(0.48-1.29) |
0.30 |
1.35 |
(0.76-1.36) |
0.27 |
1.06 |
(0.45-2.38) |
0.89 |
|
Missing data |
119 |
0.92 |
|
|
|
|
|
|
|
|
|
|
Ocular comorbidity |
4391 |
35.86 |
|
|
|
|
|
|
|
|
|
|
Pterygium on the cornea |
183 |
1.49 |
1.10 |
(0.76-1.59) |
0.61 |
1.14 |
(0.76-1.71) |
0.49 |
0.54 |
(0.24-1.13) |
0.08 |
|
Corneal opacity |
88 |
0.72 |
0.42 |
(0.27-0.66) |
<0.01 |
1.80 |
(1.08-3.00) |
0.02 |
2.45 |
(1.34-4.40) |
<0.01 |
|
Glaucoma |
882 |
6.71 |
0.62 |
(0.53-0.72) |
<0.01 |
1.34 |
(1.12-1.61) |
<0.01 |
1.82 |
(1.46-2.27) |
<0.01 |
|
Chronic uveitis |
40 |
0.33 |
0.28 |
(0.53-0.72) |
<0.01 |
3.25 |
(1.63-6.42) |
<0.01 |
2.09 |
(0.79-5.22) |
0.09 |
|
Pseudoexfoliation |
136 |
1.11 |
0.76 |
(0.52-1.12) |
0.15 |
1.16 |
(0.72-1.84) |
0.52 |
1.47 |
(0.82-2.59) |
0.16 |
|
Phacomorphic lens |
24 |
0.20 |
0.26 |
(0.11-0.61) |
<0.01 |
0.77 |
(0.18-2.71) |
0.67 |
8.51 |
(3.51-20.41) |
<0.01 |
|
Phacolytic lens |
14 |
0.11 |
0.17 |
(0.05-0.55) |
<0.01 |
1.47 |
(0.33-5.66) |
0.55 |
8.91 |
(2.74-28.25) |
<0.01 |
|
Subluxated/dislocated lens |
37 |
0.30 |
0.23 |
(0.12-0.46) |
<0.01 |
1.74 |
(0.76-3.85) |
0.15 |
5.73 |
(2.71-11.93) |
<0.01 |
|
Amblyopia |
34 |
0.28 |
0.31 |
(0.15-0.63) |
<0.01 |
3.35 |
(1.59-7.01) |
<0.01 |
1.58 |
(0.47-4.7) |
0.39 |
|
Previous eye trauma |
15 |
0.12 |
0.46 |
(0.15-1.45) |
0.13 |
1.35 |
(0.30-5.11) |
0.64 |
2.96 |
(0.62-10.23) |
0.10 |
|
NPDR |
690 |
5.64 |
0.57 |
(0.49-0.68) |
<0.01 |
1.33 |
(1.09-1.63) |
<0.01 |
2.12 |
(1.68-2.66) |
<0.01 |
|
PDR |
549 |
4.48 |
0.34 |
(0.28-0.40) |
<0.01 |
2.13 |
(1.75-2.60) |
<0.01 |
2.94 |
(2.33-3.70) |
<0.01 |
|
Maculopathy |
165 |
1.35 |
0.26 |
(0.19-0.35) |
<0.01 |
2.59 |
(1.84-3.65) |
<0.01 |
3.38 |
(2.28-5.00) |
<0.01 |
|
Vitreous haemorrhage |
88 |
0.72 |
0.08 |
(0.04-0.13) |
<0.01 |
2.03 |
(1.23-3.33) |
<0.01 |
13.54 |
(8.68-21.11) |
<0.01 |
|
ARMD |
202 |
1.65 |
0.52 |
(0.39-0.71) |
<0.01 |
1.74 |
(1.24-2.44) |
<0.01 |
1.69 |
(1.08-2.62) |
0.02 |
|
Other macular disease |
97 |
0.79 |
0.22 |
(0.14-0.34) |
<0.01 |
2.94 |
(1.89-4.56) |
<0.01 |
3.52 |
(2.12-5.82) |
<0.01 |
|
Retinal detachment |
91 |
0.74 |
0.07 |
(0.04-0.12) |
<0.01 |
1.62 |
(0.96-2.71) |
0.05 |
17.38 |
(11.17-27.07) |
<0.01 |
|
Other ocular comorbidity |
368 |
3.01 |
0.57 |
(0.46-0.71) |
<0.01 |
1.39 |
(1.07-1.82) |
0.01 |
2.00 |
(1.46-2.72) |
<0.01 |
|
Systemic comorbidity |
9330 |
76.2 |
|
|
|
|
|
|
|
|
|
|
Hypertension |
7176 |
58.61 |
1.07 |
(0.98-1.16) |
0.13 |
0.99 |
(0.90-1.10) |
0.86 |
0.86 |
(0.76-0.99) |
0.03 |
|
Diabetes mellitus |
5496 |
44.89 |
0.83 |
(0.76-0.90) |
<0.01 |
1.17 |
(1.06-1.30) |
<0.01 |
1.20 |
(1.05-1.37) |
0.01 |
|
Ischaemic heart disease |
1291 |
10.54 |
1.07 |
(0.93-1.23) |
0.37 |
0.97 |
(0.83-1.15) |
0.74 |
0.90 |
(0.71-1.13) |
0.33 |
|
Renal failure |
289 |
2.36 |
0.42 |
(0.33-0.54) |
<0.01 |
1.92 |
(1.46-2.53) |
<0.01 |
2.24 |
(1.59-3.13) |
0.00 |
|
Cerebrovascular accident |
93 |
0.76 |
0.58 |
(0.37-0.91) |
0.01 |
1.68 |
(1.01-2.77) |
0.03 |
1.43 |
(0.69-2.85) |
0.29 |
|
COPD/asthma |
429 |
3.50 |
1.29 |
(1.00-1.66) |
0.04 |
0.82 |
(0.61-1.10) |
0.17 |
0.76 |
(0.49-1.15) |
0.17 |
|
Other systemic comorbidity |
1553 |
12.68 |
1.08 |
(0.95-1.23) |
0.21 |
0.98 |
(0.85-1.14) |
0.81 |
0.84 |
(0.68-1.04) |
0.10 |
|
Previous ocular surgery |
457 |
3.52 |
0.42 |
(0.34-0.51) |
<0.01 |
1.52 |
(1.19-1.94) |
<0.01 |
3.06 |
(2.37-3.96) |
<0.01 |
|
Duration of surgery (min) |
|
|
|
|
|
|
|
|
|
|
|
|
<30 |
8837 |
68.02 |
2.13 |
(1.95-2.32) |
<0.01 |
0.55 |
(0.50-0.61) |
<0.01 |
0.46 |
(0.40-0.53) |
<0.01 |
|
31-60 |
3179 |
24.47 |
0.64 |
(0.58-0.71) |
<0.01 |
1.51 |
(1.36-1.68) |
<0.01 |
1.40 |
(1.21-62) |
<0.01 |
|
>60 |
921 |
7.09 |
0.34 |
(0.29-0.39) |
<0.01 |
1.95 |
(1.65-2.30) |
<0.01 |
3.28 |
(172-3.96) |
<0.01 |
|
Combined surgery |
617 |
4.75 |
0.36 |
(0.31-0.43) |
<0.01 |
1.52 |
(1.23-1.87) |
<0.01 |
3.85 |
(3.11-4.76) |
<0.01 |
|
Type of surgery |
|
|
|
|
|
|
|
|
|
|
|
|
Phacoemulsification |
10497 |
80.80 |
2.53 |
(2.29-2.80) |
<0.01 |
0.45 |
(0.40-0.51) |
<0.01 |
0.46 |
(0.40-0.53) |
<0.01 |
|
ECCE |
2000 |
15.39 |
0.47 |
(0.42-0.52) |
<0.01 |
2.11 |
(1.87-2.38) |
<0.01 |
1.56 |
(1.32-1.85) |
<0.01 |
|
PHACO
converted to ECCE |
185 |
1.42 |
0.51 |
(0.37-0.71) |
<0.01 |
1.74 |
1.20-2.52) |
<0.01 |
1.79 |
(1.10-2.86) |
<0.01 |
|
Lens
aspiration |
161 |
1.24 |
0.36 |
(0.25-0.50) |
<0.01 |
1.58 |
(1.04-2.41) |
0.02 |
3.69 |
(2.42-5.60) |
<0.01 |
|
ICCE |
78 |
0.60 |
0.14 |
(0.08-0.23) |
<0.01 |
2.28 |
(1.32-3.90) |
<0.01 |
7.89 |
(4.75-13.07) |
<0.01 |
|
Missing data |
71 |
0.53 |
|
|
|
|
|
|
|
|
|
Table 1 Association
between visual outcome and various patient-related factors and
procedure-related factors
(Continued)
|
Visual outcome |
Total |
% |
Good visual outcome |
Impaired visual outcome |
Poor visual outcome |
||||||
|
OR |
95%CI |
P |
OR |
95%CI |
P |
OR |
95%CI |
P |
|||
|
IOL site |
|
|
|
|
|
|
|
|
|
|
|
|
Posterior
chamber IOL |
12429 |
95.67 |
3.87 |
(0.93-5.11) |
<0.01 |
0.30 |
(0.22-0.40) |
<0.01 |
0.43 |
(0.29-0.64) |
<0.01 |
|
Anterior
chamber IOL |
170 |
1.31 |
0.26 |
(0.19-0.36) |
<0.01 |
3.39 |
(2.42-4.73) |
<0.01 |
2.29 |
(1.44-3.62) |
<0.01 |
|
Scleral-fixated
IOL |
55 |
0.43 |
0.21 |
(0.12-0.38) |
<0.01 |
3.96 |
(2.17-7.19) |
<0.01 |
2.46 |
(1.07-5.47) |
0.03 |
|
Missing data |
338 |
2.60 |
|
|
|
|
|
|
|
|
|
|
IOL type |
|
|
|
|
|
|
|
|
|
|
|
|
Foldable |
10622 |
81.76 |
2.18 |
(1.96-2.43) |
<0.01 |
0.49 |
(0.44-0.56) |
<0.01 |
0.55 |
(0.47-0.65) |
<0.01 |
|
Non-foldable |
2067 |
15.90 |
0.47 |
(0.42-0.52) |
<0.01 |
2.03 |
(1.80-2.29) |
<0.01 |
1.69 |
(1.43-2.00) |
<0.01 |
|
Missing data |
303 |
2.34 |
|
|
|
|
|
|
|
|
|
|
Intra-operative complications |
947 |
7.29 |
0.38 |
(0.33-0.43) |
<0.01 |
2.04 |
(1.74-2.40) |
<0.01 |
2.58 |
(2.12-3.14) |
<0.01 |
|
Postop. complications |
389 |
2.99 |
0.42 |
(0.32-0.55) |
<0.01 |
1.65 |
(1.21-2.25) |
<0.01 |
2.74 |
(1.94-3.85) |
<0.01 |
OR: Odds ratio; CI: Confidence interval; ECCE: Extra-capsular cataract extraction;
ICCE: Intra-capsular cataract extraction; IOL: Intraocular lens; PDR:
Proliferative diabetic retinopathy; NPDR: Non-proliferative diabetic
retinopathy; COPD: Chronic obstructive pulmonary disease; PHACO:
Phacoemulsification; ARMD:
Age-related macular degeneration.
Figure 2 displays
the gender and ethnic distribution of cataract surgery patients seen in Melaka
Hospital, 2007-2014. There were 6111 male patients (47%) and 6881 female
patients (53%). The majority of patients were Malays (47.79%), with 38.20% of
patients being Chinese and another 12.37% were Indians. Other races all
comprised less than 1% of the total population. Table 1 shows that Malays were
at an increased risk for a poor visual outcome while Chinese and Indians had a
better chance of a good visual outcome.
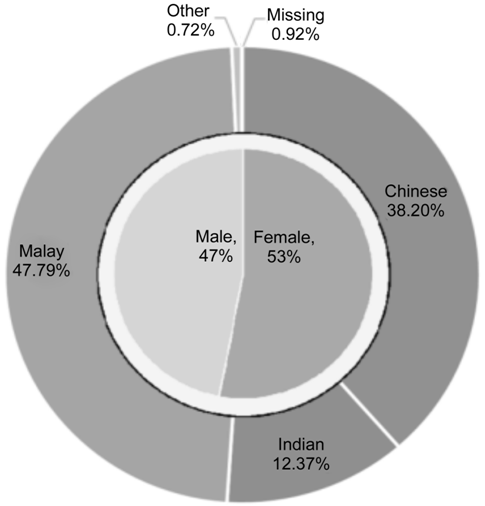
Figure 2 Gender and ethnic distribution of cataract
surgery patients at Melaka Hospital, 2007-2014.
As shown in Figure 3, the majority of patients had poor vision
preoperatively (n=7150, 55.03%), while 4213 (32.43%) had impaired
vision, and relatively few had good vision (n=1629, 12.54%) as would be
expected. The majority (98.6%) of cataracts were primary in origin, with only
1.4% being due to secondary causes. As shown in Figure 4, the majority of
secondary cataracts were due to trauma (n=101, 0.8%), with 16 drug
induced, 13 surgically induced, and another 16 due to other (unspecified)
secondary causes.
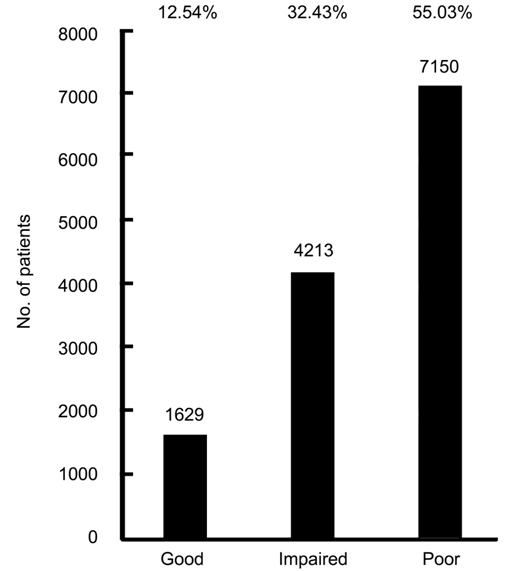
Figure 3 Preoperative visual acuity of cataract surgery patients at
Melaka Hospital, 2007-2014.
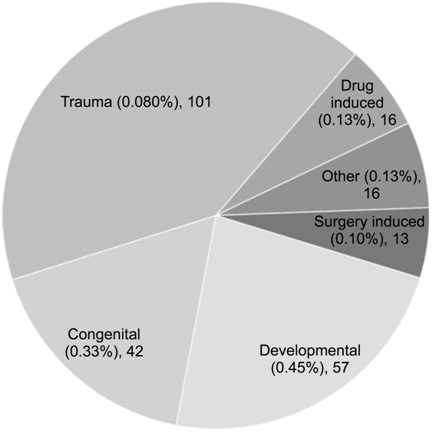
Figure 4 Aetiology of secondary cataract among cataract surgery patients
at Melaka Hospital, 2007-2014.
As many as 35.86% (n=4391) of our patients had at least one
ocular comorbidity (Table 1). The most frequent ocular comorbidities were
glaucoma (n=882, 6.71%), non-proliferative diabetic retinopathy (NPDR; n=690,
5.64%) and proliferative diabetic retinopathy (PDR; n=549, 4.48%).
Patients with these diseases all had a greater likelihood of a poorer visual
outcome. Less common ocular morbidities included age-related macular
degeneration (ARMD, n=202, 1.65%), corneal pterygium (n=183,
1.49%), maculopathy (n=165, 1.35%) and pseudoexfoliation (n=136,
1.11%).
One or more systemic comorbidities were seen in 76.2% (9330) of our
patients, the most frequent of which were hypertension (n=7176, 58.61%),
and DM (n=5496, 44.89%). There were also 1553 cases of other unspecified
comorbidities (12.68%), 1291 patients with ischemic heart disease (10.54%), 429
patients with chronic obstructive pulmonary disease/ asthma (3.50%), 289 cases
of renal failure (2.36%), and 93 patients had suffered a previous
cerebrovascular accident (0.76%). Hypertension (P=0.03) and diabetes (P=0.01)
affected visual outcomes.
Trends in
surgical duration suggested that shorter surgeries (less than 30min) were 2.13
times more likely to be associated with a ‘good’ visual outcome (P<0.01), compared to an OR of 0.64
and 0.34 for surgeries that lasted 31-60min and >60min, respectively.
Conversely, surgeries that lasted >60min were 3.28 times more likely to result in a ‘poor’ visual outcome (P<0.01).
Combined
surgeries were associated with a significantly higher chance of a poor outcome
(OR: 0.36, P<0.01).
Overall, phacoemulsification was
significantly associated with a ‘good’ visual outcome (OR: 2.53, P<0.01), while other methods were shown to lower the chances of
a ‘good’ visual outcome. The chance of a ‘poor’
visual outcome was high after an intra-capsular cataract extraction (ICCE) (OR:
7.89) and lens aspiration (OR: 3.69).
The type of
the IOL was also found to significantly affect the visual outcome. A posterior
chamber intraocular lens (PCIOL) was
more strongly associated with a ‘good’ visual outcome (OR: 3.87) than an
antenior chamber intraocular lens (ACIOL) (OR: 0.26) or a scleral-fixed IOL
(OR: 0.21), which were associated with a greater likelihood of a ‘poor’ visual outcome (OR: 2.29 and 2.46, respectively). Foldable
lenses increased the likelihood of a ‘good’ visual outcome (OR: 2.18), while non-foldable lenses predisposed to
a ‘poor’ visual outcome (OR: 1.69). Both intra-operative and post-operative
complications were associated with a greater risk of a ‘poor’ visual outcome (OR: 2.58 and 2.74, respectively).
DISCUSSION
We found that the demographic makeup of our patients comprised of Malays
(47.79%), Chinese (38.20%), and Indians (12.37%), which roughly represented the
ethnic distribution of the Melakan population. Gender distribution was fairly
equal between males (47%) and females (53%). Chinese generally had better
outcomes than Malays. Extremes of age were associated with lower chances of
good outcomes, a finding which is corroborated by Schein et al[7].
Preoperatively as many as 7150 (55.03%) eyes had poor vision of 6/60 and
worse. In a Malaysian district hospital study, Thevi et al[8] found that cataract (248, 22.9%) was the most common
eye disease, accounting for severe visual impairment in 11 out of 12 patients.
Reddy et al[9] found that cataract
(385, 32.9%) was the most common eye disease in urban population in Malaysia.
The majority of patients had primary cataracts (98.6%). Paediatric
patients presented with congenital cataract in 42 cases (0.33%) and
developmental cataract in 57 (0.45%). This group should undergo surgery as soon
as possible to prevent amblyopia (lazy eye). Doctors should be alert to examine
the eyes of newborn and younger aged individuals to look for the red reflex and
in its absence, to refer early for intervention. Due to screening procedures
with a hand held ophthalmoscope for red reflex examination in Swedish Maternity
Wards, congenital cataracts are referred earlier in Swedish children compared
to Danish children[10]. Age at
cataract extraction significantly affects the visual outcome in paediatric
cataracts. Health workers and school teachers could be trained to use Snellen
charts to test children’s vision, as in Nepal[11].
Drug induced cataracts were also reported; Steroids are known to cause
cataracts and patients should be informed of this possible complication to
enable early reporting and secondary prevention. In the USA, recent approvals
have made intranasal steroids available over-the-counter (OTC), raising concern
that genetically sensitive individuals may develop lens opacities[12].
Phacomorphic (0.20%) and phacolytic (0.11%) lenses were also seen in our
patients. Although access for ocular treatment is available, patients still
present at a very late stage for cataract surgery. For patients with such
advanced cataracts, lens-induced glaucoma is a very pressing problem, as a
recent study reported that 2.4% of 12 004 cataract patients experienced it at
presentation[13]. Vision in such patients is very
poor; a Malaysian study found that 84.2% of 38 eyes with lens-induced glaucoma
presented with only hand movement vision[14].
Screening measures must be instituted to prevent this.
Glaucoma, NPDR and PDR were the commonest ocular comorbidities at
presentation, and were also associated with poorer outcomes.
Cataract surgery has been found to successfully reduce medications
required for glaucoma management[15]. Toric
IOLs reduced astigmatism and improved vision among glaucoma patients undergoing
cataract surgery[16]. Ophthalmologists and family
doctors should discuss this benefit for patients with cataract and glaucoma who
are unsure about the benefits of cataract surgery. We found that ocular
comorbidities and previous ocular surgeries reduced the likelihood of obtaining
good visual outcomes.
With dense cataracts, comorbidities in the posterior segment (e.g.
ARMD, vitreous haemorrhage, retinal detachment and maculopathy and macular
disease) are sometimes invisible, and not all can be diagnosed with B-scan
ultrasonography. Patients must be told about the existence of such
comorbidities and the guarded prognosis or the need for further intervention
should they be present. Lai et al[17]
found that ARMD and vitreous loss were associated with lower chance of visual
improvement among elderly. Jammal et al[18]
found that ARMD and diabetic maculopathy were the most common causes of reduced
visual acuity following phacoemulsification in obscured fundus view. Analysis
from the National Cataract Swedish Register found that ocular comorbidity was
related to no benefit outcome after cataract surgery[19].
In Malaysia, diabetic eye disease is the commonest cause of visual loss
in the adult working age group[20]. In
a study in University Malaya Medical Center, 29.2% of type 2 diabetic patients
presented with diabetic retinopathy findings on the first visit[21]. Higher risks of complications, such as
worsening of diabetic retinopathy and macula oedema following cataract surgery, are seen among diabetics[22].
Smalling and others found that diabetics with advanced age on insulin had
decreased postoperative visual acuity and visual functions which affected the
quality of life[23]. The use of
intravitreal triamcinolone or bevacizumab at the time of cataract surgery was
found to benefit patients with pre-existing macular edema or moderate-to-severe
NPDR[24]. A cochrane[25]
review however, found low quality evidence for the efficacy and safety of
anti-vascular endothelial growth factor (VEGF) agents when used to treat PDR
over and above current standard treatments. Early detection and
treatment options for such cases should be discussed by the physician and
ophthalmologist.
A variety of systemic comorbidities were present during presentation for
cataract surgeries, the most common of which were hypertension and diabetes. A
Meta-analysis found that the risk of cataracts in hypertensive populations was
significantly higher among cohort studies[26].
Physicians treating these systemic disorders should perform routine ocular
examinations to detect cataracts and refer suspected cases to prevent mature
cataracts. Hypertension and tamsulosin therapy have been significantly
associated with intraoperative floppy iris syndrome[27].
The treating physician should mention these conditions in the referral so
that the operating surgeon will be aware of the difficulties that may arise due
to floppy iris. Cerebrovascular accidents present with a variety of field
defects which may be the only presenting symptom[28].
Patients should be informed prior to cataract surgery about the possibility of
persistent visual field defects, so as not to expect full recovery
post-operatively. Renal failure patients should be prescribed relevant drugs
with caution, and dialysis should be scheduled appropriately around surgery.
William et al[29] described a patient with
diabetes, renal failure and recent cataract surgery who developed severe
intraocular hypertension during dialysis. Nephrologists and staff in
dialysis centres should be aware of this.
Duration of
surgeries affected the visual outcomes in our study. Surgeries completed within
30min produced better outcomes compared to longer duration surgeries. Complex
surgeries take a longer time to do, and this could be a possible explanation
about poorer outcomes in longer duration surgeries. However, Thanigasalam et al[30] found that the duration of surgery did not affect the visual
outcomes. Combination
surgeries were associated with poorer outcomes. This could be due to either the
pre-existing comorbidities which were already a factor for poorer outcomes or
due to further complications developing. Combination surgeries in our center
are filtering surgeries or glaucoma drainage device surgeries or vitreoretinal
surgeries which are done along with cataract surgeries. In a study of combined
and sequential surgeries of phacoemulsification and vitrectomy in PDR, there
was a higher incidence of fibrinous exudation in the combined surgery group[31]. Several other studies found no difference between combination
and sequential surgeries for cataract and vitrectomies[32]. Kim et al[33] found good outcomes following combined cataract and retinal
detachments surgeries in macula on cases. Tzu et al[34] noted good outcomes in combination surgeries of simultaneous cataract extraction with
trabeculectomy or glaucoma drainage device surgery. Similar to other studies, we too found that phacoemulsification
gave the best visual outcomes compared to other techniques[35].
Foldable
PCIOLs were associated with a higher chance of good outcomes than other lenses. However, some studies[36-37] challenge this finding. In our setup, when posterior capsular support is inadequate,
ACIOLs and scleral-fixated IOLs are used. We found that ACIOLs had better
outcomes than scleral-fixated IOL, as have other studies[38]. However, a
study[39] by the
American Academy of Ophthalmology found no difference in outcome between these
two lenses. Intraoperative
and postoperative complications were associated with poorer outcomes - a
finding corroborated by Yuan et al[40]. However, in a study of 1632 cases, Thanigasalam et al[30] concluded that intraoperative
complications did not affect visual outcomes.
In conclusion, primary care physicians have a role to screen and detect
patients for cataract to prevent the late presentation causing blindness. They
should adequately control the systemic disorders as comorbidities affect
outcomes. Community screening measures and public health education should
ensure that patients present earlier, to prevent blindness and facilitate
timely surgery. Patients who request less expensive options should be counseled
on the benefits of phacoemulsification over other surgical techniques, and the
advantages of a foldable IOL. Meticulous
care should be taken to avoid operative complications. However, should these
occur, surgeons should preferably use an ACIOL rather than a scleral-fixated
IOL.
ACKNOWLEDGEMENTS
We thank the Director General of Health Malaysia for permission to
publish.
Conflicts of
Interest: Thevi T, None; Godinho MA, None.
REFERENCES
1 Zainal M,
Ismail S, Ropilah A, Elias H, Arumugam G, Alias D, Fathilah J, Lim TO, Ding LM,
Goh PP. Prevalence of blindness and low vision in Malaysian population: results
from the National Eye Survey 1996. Br J
Ophthalmol 2002;86(9):951-956. [CrossRef] [PubMed]
2 Wortz G. Reducing
liability risk through informed consent. The Journal of medical practice
management: MPM 2011;26(4):203. [PubMed]
3 Cornut PL,
Thuret G, Creuzot-Garcher C, Maurin M, Pechinot A, Bron A, Gain P, Carricajo A,
Denis P, Romanet JP, Vandenesch F, Chiquet C; French Institutional
Endophthalmitis Study Group. Relationship between baseline clinical data and
microbiologic spectrum in 100 patients with acute postcataract endophthalmitis.
Retina 2012;32(3):549-557. [CrossRef] [PubMed]
4 Agarwal
PK, Mathew M, Virdi M. Is there an effect of perioperative blood pressure on
intraoperative complications during phacoemulsification surgery under local
anaesthesia? Eye (Lond) 2010;24(7):1186-1192. [CrossRef] [PubMed]
5 Feldman-Billard
S, Sedira N, Boelle PY, Poisson F, Héron E. High prevalence of undiagnosed
diabetes and high risk for diabetes using HbA1c criteria in middle-aged
patients undergoing cataract surgery. Diabetes
Metab J 2013;39(3):271-275. [CrossRef] [PubMed]
7 Schein OD,
Steinberg EP, Cassard SD, Tielsch JM, Javitt JC, Sommer A. Predictors of
outcome in patients who underwent cataract surgery. Ophthalmology 1995;102(5):817-823. [CrossRef]
8 Thevi T,
Basri M, Reddy S. Prevalence of eye diseases and visual impairment among the
rural population-a case study of temerloh hospital. Malays Fam Physician 2012;7(1):6-10. [PMC free article] [PubMed]
9 Reddy S,
Tajunisah I, Low K, Karmila A. Prevalence of eye diseases and visual impairment
in urban population-a study from University of Malaya Medical Centre. Malays Fam Physician 2008;3(1):25-28. [PMC free article] [PubMed]
10 Haargaard
B, Nyström A, Rosensvärd A, Tornqvist K, Magnusson G. The Pediatric Cataract
Register (PECARE): analysis of age at detection of congenital cataract. Acta Ophthalmologica 2015;93(1):24-26. [CrossRef] [PubMed]
11 Adhikari
S, Shrestha MK, Adhikari K, Maharjan N, Shrestha UD. Causes of visual
impairment and blindness in children in three ecological regions of Nepal:
Nepal Pediatric Ocular Diseases Study. Clin
Ophthalmol 2015;9:1543-1547. [CrossRef] [PMC free article] [PubMed]
12 Bielory B,
Bielory L. Over-the-counter migration of steroid use: impact on the eye. Curr Opin Allergy Clin Immunol 2014;14(5):471-476. [CrossRef] [PubMed]
13 Kothari
R, Tathe S, Gogri P, Bhandari A. Lens-induced glaucoma: the need to spread
awareness about early management of cataract among rural population. ISRN Ophthalmol 2013;2013:581727. [CrossRef] [PMC free article] [PubMed]
14 Yaakub A,
Abdullah N, Siti Raihan I, Ahmad Tajudin LS. Lens-induced glaucoma in a tertiary
centre in northeast of Malaysia. Malays
Fam Physician 2014;9(2):48-52. [PMC free article] [PubMed]
15 Hayashi
K, Hayashi H, Nakao F, Hayashi F. Effect of cataract surgery on intraocular
pressure control in glaucoma patients. J
Cataract Refract Surg 2001;27(11):1779-1786. [CrossRef]
16 Brown RH,
Zhong L, Bozeman CW, Lynch MG. Toric intraocular lens outcomes in patients with
glaucoma. J Cataract Refract Surg 2015;31(6):366-372. [CrossRef] [PubMed]
17 Lai FH,
Lok JY, Chow PP, Young AL. Clinical outcomes of cataract surgery in very
elderly adults. J Am Geriatr Soc 2014;62(1):165-170.
[CrossRef] [PubMed]
18 Jammal
HM, Khader Y, Shawer R, Al Bdour M. Posterior segment causes of reduced visual
acuity after phacoemulsification in eyes with cataract and obscured fundus
view. Clin Ophthalmol 2012;6:1843-1848. [CrossRef] [PMC free article] [PubMed]
19 Lundström
M, Stenevi U, Thorburn W. Outcome of cataract surgery considering the
preoperative situation: a study of possible predictors of the functional
outcome. Br J Ophthalmol
1999;83(11):1272-1276. [CrossRef]
21 Tajunisah
I, Wong PS, Tan LT, Rokiah P, Reddy SC. Awareness of eye complications and
prevalence of retinopathy in the first visit to eye clinic among type 2
diabetic patients. Int J Ophthalmol 2011;4(5):519-524. [PMC free article] [PubMed]
22 Flesner
P, Sander B, Henning V, Parving HH, Dornonville de la Cour M, Lund-Andersen H.
Cataract surgery on diabetic patients. A prospective evaluation of risk factors
and complications. Acta Ophthalmol Scand 2002;80(1):19-24. [CrossRef]
23
Lara-Smalling A, Cakiner-Egilmez T. Diabetes and cataract surgery: preoperative
risk factors and positive nursing interventions. Insight 2014;39(2):18-20. [PubMed]
24
Gallego-Pinazo R, Dolz-Marco R, Berrocal M, Wu L, Maia M, Serrano M,
Alezzandrini A, Arévalo JF, Díaz-Llopis M; Pan-American Collaborative Retina
Study Group (PACORES). Outcomes of cataract surgery in diabetic patients:
results of the Pan American Collaborative Retina Study Group. Arq Bras Oftalmol 2014;77(6):355-359. [CrossRef] [PubMed]
25
Martinez-Zapata MJ, Marti-Carvajal AJ, Solà I, Pijoán JI, Buil-Calvo JA,
Cordero JA, Evans JR. Anti-vascular endothelial growth factor for proliferative
diabetic retinopathy. Cochrane Database
Syst Rev 2014;11:CD008721. [CrossRef]
26 Yu X, Lyu
D, Dong X, He G, Yao K. Hypertension and risk of cataract: a meta-analysis. PLoS One 2014;9(12):e114012. [CrossRef] [PMC free article] [PubMed]
27 Goyal S,
Dalela D, Goyal NK, Chawla S, Dhesi R, Kamboj B, Dalela A. Intraoperative floppy
iris syndrome in Indian population: a prospective study on incidence, risk
factors, and impact on operative performance. Indian J Ophthalmol 2014;62(8):870-875. [CrossRef] [PMC free article] [PubMed]
29 William
JH, Gilbert AL, Rosas SE. Keeping an eye on dialysis: the association of
hemodialysis with intraocular hypertension. Clin
Nephrol 2015;84(5):307-310. [CrossRef] [PubMed]
30 Thanigasalam
T, Reddy SC, Zaki RA. Factors associated with complications and postoperative
visual outcomes of cataract surgery; A study of 1632 cases. J Ophthalmic Vis Res 2015;10(4):375-384.
[CrossRef] [PMC free article] [PubMed]
31 Yang Y,
Zhang J, Yan H. Comparison of combined and sequential surgery for proliferative
diabetic retinopathy: a single surgeon study. PLoS One 2014;9(9):e108933. [CrossRef] [PMC free article] [PubMed]
32 Chung TY,
Chung H, Lee JH. Combined surgery and sequential surgery comprising
phacoemulsification, pars plana vitrectomy, and intraocular lens implantation:
comparison of clinical outcomes. J
Cataract Refract Surg 2002;28(11):2001-2005. [CrossRef]
33 Kim KN,
Lee HJ, Heo DW, Jo YJ, Kim JY. Combined cataract extraction and vitrectomy for
macula-sparing retinal detachment: visual outcomes and complications. Korean J Ophthalmol 2015;29(3):147-154. [CrossRef] [PMC free article] [PubMed]
34 Tzu JH,
Shah CT, Galor A, Junk AK, Sastry A, Wellik SR. Refractive outcomes of combined
cataract and glaucoma surgery. J Glaucoma
2015;24(2):161-164. [CrossRef] [PubMed]
35 Thevi T,
Reddy SC, Shantakumar C. Outcome of phacoemulsification and extracapsular
cataract extraction: a study in a district hospital in Malaysia. Malays Fam Physician 2014;9(2):41-47. [PMC free article] [PubMed]
36 Hennig A,
Puri LR, Sharma H, Evans JR, Yorston D. Foldable vs rigid lenses after
phacoemulsification for cataract surgery: a randomised controlled trial. Eye (Lond) 2014;28(5):567-575. [CrossRef] [PMC free article] [PubMed]
37 Afsar AJ,
Patel S, Woods RL, Wykes W. A comparison of visual performance between a rigid
PMMA and a foldable acrylic intraocular lens. Eye (Lond) 1999;13(Pt 3a):329-335. [CrossRef] [PubMed]
38 Dadeya S,
Kamlesh, Kumari Sodhi P. Secondary intraocular lens (IOL) implantation:
anterior chamber versus scleral fixation-long-term comparative evaluation. Eur J Ophthalmol 2003;13(7):627-633. [PubMed]
39 Wagoner
MD, Cox TA, Ariyasu RG, Jacobs DS, Karp CL; American Academy of Ophthalmology.
Intraocular lens implantation in the absence of capsular support: a report by
the American Academy of Ophthalmology. Ophthalmology
2003;110(4):840-859. [CrossRef]
40 Yuan J,
Wang X, Yang LQ, Xing YQ, Yang YN. Assessment of visual outcomes of cataract
surgery in Tujia nationality in Xianfeng County, China. Int J Ophthalmol 2015;8(2):292-298. [PMC free article] [PubMed]
--------------------------------------------------------------------------------------------------------------------------------
All rights reserved by Press of International Journal of Ophthalmology (IJO
PRESS)